In this Article
Melanoma
What Is Melanoma?
Melanoma is a rare but potentially serious type of skin cancer.
Skin cancer is a disease in which skin cells lose the ability to divide and grow normally. These abnormal skin cells can grow and form a mass or “tumor.”
A skin tumor is considered benign (not cancer) if it is limited to a few cell layers and does not invade surrounding tissues or organs. If the tumor spreads to surrounding tissues, it is considered malignant, or cancerous. Cancer cells crowd out and destroy nearby healthy cells, forming growths called malignant tumors.
Most skin growths are benign tumors. However, melanoma is a malignant skin growth because it can
Malignant melanoma has a very high cure rate if diagnosed early and treated promptly.
Melanoma that spreads to vital organs like the brain or liver can be life-threatening.
Understanding how melanoma develops:
The skin is made up of 3 layers:
- The
epidermis , or outer layer of skin, which is made up of three different types of cells - The
dermis , or middle layer of the skin; it contains nerves, blood vessels, sweat glands, hair follicles, and oil-producing cells that keep the skin from drying out - The fatty layer

The epidermis in made up of 3 different types of cells. Different types of skin cancer are named for the kind of cell that becomes malignant.
Basal cell carcinoma starts in basal cells, which are small, round cells found at the base of the epidermis. It is the most common kind of skin cancer. More than 90 percent of all skin cancers in the United States are basal cell carcinomas. Basal cell carcinoma is the least serious kind of skin cancer because it grows slowly and seldom spreads.Squamous cell carcinoma starts in squamous cells, which are flat scaly cells that form the outermost part of the skin. Squamous cell carcinoma is more serious because it spreads more often than basal cell carcinoma. However, squamous cell carcinoma usually spreads slowly.- Melanoma starts in the
melanocytes , which are pigment-producing cells found mainly in the lower part of the epidermis (the outer layer of the skin). They make a dark material, melanin, which gives skin its natural color. Melanoma is serious because the malignant cells tend to spread rapidly from the skin to internal organs.
|
Melanomas may form from an existing mole or freckle, or begin to grow from a normal-appearing area of the skin. |
|
Melanomas vs. normal moles:
|
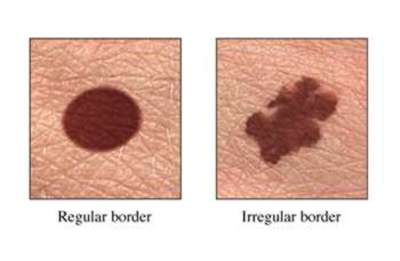
|
Melanomas often show the ABCD symptoms:
|
|
If a mole changes size or appearance, or bleeds, or becomes a wound that does not heal then you must have this looked at by a doctor as it may be a sign of cancer. |
|
Your chances of finding skin cancer can be improved by performing a regular skin examination at home. Follow these tips:
By checking your skin regularly, you will become familiar with what is normal. If you find anything unusual, see your doctor right away. Remember, the earlier skin cancer is found, the better the chance for cure. The following self-exam routine should take no more than 15 minutes:
|
|
Nice To Know: Q. My mother had melanoma. I’m worried that I may get it, too, especially because I have a lot of moles on my skin. What kind of medical checkups are recommended? A. Melanoma does run in families. If your parents had melanoma, your own risk may be higher than normal – especially if you have many moles of a certain kind. Your primary care doctor should do a total skin examination at each routine physical examination. That involves inspecting every inch of your skin, including the genital region and the area between the buttocks. If the doctor spots suspicious growths, you’ll probably get a referral to a |
Although most pigment-producing cells are in the skin, some of these types of cells occur in other parts of the body and can also become malignant. For example,
|
Facts About Melanoma
|
Who is most at risk of developing melanoma?
Anyone can get melanoma. Certain individuals, however, have several risk factors for melanoma. They are at higher risk for getting the disease than the general population. But risk factors do not cause a disease. Many people with risk factors for melanoma never get the condition.
People with higher-than-normal risk include those who have or have had:
- Many moles: Individuals who have certain types of moles, typically bigger than ordinary moles (also called ‘dysplastic nevi’), are at a greater risk of developing
malignant melanoma. To learn more about moles see What are moles? - Family history of melanoma: Having parents or siblings who have had malignant melanoma increases a person’s risk. A person with dysplastic nevi and at least two close relatives with melanoma has a 50 percent higher risk of developing melanoma.
- Personal history of melanoma: A person who has had melanoma before may get it again in a different part of the skin. Melanoma that was treated also may
recur . - Sun exposure: People who work or spend lots of leisure time outside are at increased risk for all skin cancers. People who live at higher elevations are also at greater risk because the atmosphere is thinner and does not filter UV rays as well.
- Sunburn: Having one or more blistering sunburns before the age of 20 increases risk for developing melanoma later in life. Severe sunburns in adults also increase risk.
- Immune suppression drugs: The body’s immune system detects and destroys cancer cells. Immune suppression drugs may weaken this protective action. Drugs used to prevent rejection of transplanted organs and treat cancer are among those that suppress the immune system.
- Advanced age: Almost half of all melanoma cases are diagnosed in individuals age 50 and over. Yet melanoma is also one of the most common cancers diagnosed in people under 35.
What Is Your Personal Risk?
Use this skin type table to determine your susceptibility to skin cancer:
|
SKIN TYPE(Fitzpatrick) |
*RESPONSE TO SUN EXPOSURE |
EXAMPLES |
SUSCEPTIBILITY |
|
I |
Always sunburn, don’t tan |
Fair-skinned & freckled |
Very High |
|
II |
Always sunburn tan minimally |
Fair-skinned, blonde haired, Blue-eyed, Scandinavians |
High |
|
III |
Sometimes sunburn, tan moderately |
Fair-skinned, brown hair, brown-eyed; unexposed skin is white |
Average |
|
IV |
Seldom sunburn, tan easily |
Light brown skin, dark brown hair, brown-eyed; unexposed skin is tan; Mediterranean, Hispanic |
Low |
|
V |
Rarely sunburn, tan profusely |
Dark brown skin; Mediterranean, Asian, Eastern Indian |
Very low |
|
VI |
Never sunburn, Deeply pigmented |
Black |
Minimal |
* Generally based on first exposure to sun following a long period without exposure
