In this Article
Knee Replacement
What Is Knee Replacement?
Total knee replacement (TKR), also referred to as total knee arthroplasty (TKA), is a surgical procedure where worn, diseased, or damaged surfaces of a knee joint are removed and replaced with artificial surfaces. Materials used for resurfacing of the joint are not only strong and durable but also optimal for joint function as they produce as little friction as possible.

The “artificial joint or prosthesis” generally has two components, one made of metal which is usually cobalt -chrome or titanium. The other component is a plastic material called polyethylene.

The procedure has been proven to help individuals return back to moderately challenging activities such as golf, bicycling, and swimming. Total knees are not designed for jogging, or sports like tennis and skiing (although there certainly are people with total knee replacements that participate in such sports).
The general goal of total knee replacement is designed to provide painless and unlimited standing, sitting, walking, and other normal activities of daily living
|
Nice To Know: With proper care individuals who have had a total knee replacement can expect many years of faithful function. Studies show that patients can expect a greater than 95 percent chance of success for at least 15 years. |
|
If You Are Considering Total Knee Replacement Surgery If you have been told you have a severely damaged knee joint and would benefit from a total knee replacement, the questions you need to ask yourself are:
If the answesr to these questions are yes, you may be a candidate for a new knee. |
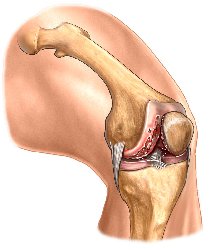
The Anatomy Of The Knee Joint

The knee joint performs similar to a hinge joint. It consists of three bones:
- Thigh bone (Femur)
- Leg bone (Tibia)
- Knee cap (Patella)
- The junction where the femur and tibia couple together is called the femorotibial joint.
- The region of the knee where the patella and femur form a junction is called the patellofemoral joint.
- These two joints are what allow the bending and straightening of the knee. It is these joints that are replaced in a total knee joint replacement.
For a knee to function normally, the quality of smoothness where each bone moves upon the other becomes important in the function of the knee joint.
The surfaces of all three bones coming into contact with each other are normally covered with a smooth gliding surface known as
The condition of this cartilage lining the knee joint is a key aspect of normal knee function and is important to the physician when evaluating a potential need for a knee joint replacement.
In addition to the smooth cartilage lining on the joint surfaces, there are two smooth discs of cartilage that cushion the space between the bone ends. The inner disc is called the medial

Generally speaking, there are four major ligaments that play an important part in stability of the knee joint. One on each side of the knee (but actually outside the joint) known as collateral ligaments and two more centrally located ligaments within the joint known as anterior and posterior cruciate ligaments.
|
Facts About Total Knee Replacement
|
What Causes The Knee Joint To Degenerate?
Any condition affecting the knee that causes damage to the normally smooth lining cartilage of the knee may eventually end up with the same end result. The protective cartilage lining the joint becomes worn away, producing increasing damage to the bone surfaces inside the joint. This may cause pain, swelling and stiffness, as the exposed bone ends grind painfully against each other.

Osteoarthritis resulting from “wear and tear” is the most common reason individuals need to undergo knee replacement surgery. This condition may be due to an old injury or infection to the knee joint, but mostly there is no obvious cause as to why this happens. The major problem in osteoarthritis of the knee joint is that the smooth cartilage lining the inside of the joint wears away. This results in a narrowing of the joint space with the development of cysts and erosions in the bone ends. As a result, bone comes directly in contact with bone, which will be painful. Bone spurs (small bone growths) form around the joint. All of these changes ultimately lead to increasing pain and stiffness of the joint.

For further information about osteoarthritis, go to Osteoarthritis.
Rheumatoid arthritis, an inflammation of the tissue surrounding the joints, can cause deterioration of cartilage and other parts of the joint and result in the need for knee joint replacement. It is one of the inflammatory types of arthritis that may affect other areas of the body such as skin, kidneys and spleen. Rheumatoid arthritiscan also affect other joints including hands, feet, elbows, hips etc.
Post-traumatic arthritis, a type of arthritis that can arise following an injury to the joint cartilage or through damage to the ligaments leading to an unstable knee. Generally speaking, any abnormalities causing excessive wear within the joint (from fractures of the knee, torn cartilage, and torn ligaments) can lead to degeneration long after the original injury and ultimately result in the need for a knee replacement.
Malalignment of the knee joint – knock-knees or bowlegs – results from an excessive angle where the upper and lower leg bones meet at the knee joint. The result is abnormally high stress on either the outer half or inner half of the joint.

Who Is A Candidate For Knee Replacement?
Total knee replacements are usually performed on people suffering from painful arthritic conditions of the knee severe enough to limit one’s normal day to day activities.
|
Need To Know: Generally a person would be considered for a total knee replacement if the individual experiences daily pain, restricting not only work and recreation, but also the ordinary activities of daily living. There must also be evidence of significant destruction of the knee as seen on an x-ray. |
Most people who have artificial knees are over age 55, but the procedure is also offered to younger people with knee degeneration if their quality of life is severely affected.
Determining the need for a total knee replacement

The diagnosis is made by:
- A complete history andphysical examination: this allows the physician to determine any correlation between symptoms of pain with past history and demands that have been placed upon the knee. The physician will also inquire about experiencing episodes of instability. The examination should focus on the assessment of swelling, range of motion, ligament stability, and knee alignment.
- X-rays are used to show the extent of damage to the joint and they may suggest a cause for the degeneration.
- Blood tests may be required to rule out inflammatory arthritis (such as Rheumatoid Arthritis) or infection in the knee if there is reason to believe that these conditions are contributing to the degenerative process..
Different Types Of Knee Replacements
Broadly speaking, there are four basic categories of knee replacements depending on the degree of mechanical stability provided by the design of the artificial knee:
The highly successful non-constrained implant is the most common type of artificial knee. It is termed non-constrained because the artificial components inserted into the knee are not linked to each other and have no stability built into the system. It relies on the person’s own ligaments and muscles for stability. This is the key feature of this group of artificial implants helping to maintain the stability of the knee.
The semi-constrained implant is a device that provides increasing stability for the knee. This type of artificial knee has some stability built into it. It is used if the surgeon needs to remove all of the inner knee ligaments(some surgeons prefer to do this), or if the surgeon feels the new knee will be more stable with this type of implant.
Constraint or hinged variety implants are rarely used as a first choice of surgical options. In this case, the two components of the knee joint are linked together with a hinged mechanism. This type of knee replacement is used when the knee is highly unstable and the person’s ligaments will not be able to support the other type of knee replacements. It is useful in the treatment of severely damaged knees particularly in very elderly people undergoing a revision replacement procedure. The disadvantage of this type of knee joint is that it is not expected to last as long as the other types.
A unicondylar knee replacement replaces only half of the knee joint. It is performed if the damage is limited to one side of the joint only with the remaining part of the knee joint being relatively spared. It is now possible for the surgeon to replace only that area of the knee joint which is severely damaged. However, even with only half of the joint destroyed, many surgeons prefer doing a total knee replacement believing this is a better procedure than the half-knee (unicondylar) replacement. But equally, there are surgeons who believe it is more appropriate to perform a unicondylar knee in the right circumstance.
How Is The Artificial Implant Fixed To Bone?
Options available that hold the knee replacement into position:
With a cemented procedure the components of the implant are fixed to the bone with a grout-like cement known as polymethyl-methacrylate. This cement allows the implants to perfectly fit to the irregularities of the bone.
A cemented knee is a very reliable procedure with approximately 90to 95 percent expected to enjoy pain-free activities for at least ten years beyond surgery. The advantage is that this type of knee replacement is immediately stable and one can walk fully bearing weight immediately following surgery. The disadvantages are that if it should become loose, some bone may be ground away by the loosened cement potentially making revision more difficult.
In a non-cemented procedure, components of the implant have a roughened porous surface designed to allow bone to grow into it, eliminating the need for cement.
The implants are “press fit” against the bony surfaces that are precisely cut through the use of multiple cutting jigs. Faultless positioning is necessary for bony attachment to occur with initial fixation by metal pegs and screws of the implant to bone. Since this implant relies on the bone to hold it in place, this procedure requires good bone to be successful
Since the non-cemented procedure is relatively new, years of experience and studies are not available regarding this type of implant as compared to the cemented implant. Therefore, at this time it is not yet known if a non-cemented implant will be as successful or will last as long as the cemented type.
One potentially positive aspect is that if this implant should become loose, less bone loss may occur due to the lack of the irritant cement. After surgery the individual with this type of implant is usually instructed to be toe-touch only until a follow-up x-ray usually done by the fifth or sixth week after surgery. The weight-bearing status following non-cemented knee replacement will be determined by the surgeon.
Occasionally a hybrid fixation is used which consists of a combination of the cemented and non-cemented technique. In this method the femoral component is not cemented and the tibia component is cemented.
At present, cemented knee replacements are most commonly used, representing 90% of knee replacement surgery. Non-cemented replacements are much less common, as are hybrid replacements.
Possible Risks And Complications
As with all major surgical procedures, complications can occur. Some of the most common complications following knee replacement are:
Deep Venous Thrombosis (DVT)
This term refers to the formation of blood clots (called thrombosis) in the large veins, usually of the legs or pelvis. It can occur after any operation, but is more likely to occur following surgery on the hip, pelvis, or knee. It results from the slowing of the blood flow in the leg during and after surgery.
A Deep Venous Thrombosis (DVT) may cause the leg to:
- Swell
- Become warm to the touch
- Become painful
|
Nice to Know: Surgeons take preventing DVT very seriously. Some of the commonly used preventative measures include:
|
For further information about deep vein thrombosis, go to Deep Vein Thrombosis.
Infection
The chance of getting an infection following artificial knee replacement is less than one percent. Some infections may show up very early, even before discharge from the hospital. Others may not become apparent for months, or even years, after the operation. All patients receive antiobiotics for at least 24 hours after surgery to minimize the risk of infection.
Infection can spread into the artificial joint from other infected areas of the body.
Therefore, your surgeon may want to make sure that you
- Take antibiotics if ever you have dental work, or undergo a surgical procedure on your bladder and colon to reduce the risk of spreading germs to the knee replacement joint.
- To minimize the risk of infection, most surgeons will defer doing total knee replacement if there is an open wound anywhere on the body.
Stiffness
To be able to use the knee effectively to rise from a chair, the replaced joint must bend at least to 90 degrees. Most surgeons desire range of motion greater than 110 degrees. In some cases, the ability to bend the knee does not return to normal after an artificial knee replacement. Because of this many surgeons utilize
- Physical therapy beginning immediately after the surgery to help regain range of motion.
- Continuous passive motion (CPM): This involves the use of a specialized machine immediately after surgery to increase the range of motion of the operated knee following artificial knee replacement.
Occasionally, excessive scarring after surgery can lead to an increasingly stiff knee. If this occurs, the surgeon may recommend taking the individual back to the operating room after the surgery and simply manipulate ( i.e. bend) the knee under anesthesia to regain motion. This allows the surgeon to breakup and stretch the scar tissue to increase the motion in the knee without injuring the joint.
The most important factor in preventing stiffness is keeping the knee moving in the days and weeks following surgery and actively participating in the physical therapy program.
Loosening
The major reason artificial joints may eventually fail is because of loosening where the metal or cement meets the bone. There have been great advances in extending how long an artificial joint will last, but loosening is a possibility that may require a revision.
Today one can expect 12-15 years or more of service from an artificial knee. However, in some cases the knee will loosen earlier. A loose artificial implant becomes a problem because of pain and wearing away of the bone. If loosening occurs, another knee replacement may need to be done (this is called a revision total knee replacement). Therefore it is sensible for the individual to have yearly follow up visits with their surgeon that will include an x-ray evaluation of the operated knee.
Osteolysis
A complication that can cause the artificial components to loosen or damage the bone is called osteolysis meaning “breakdown of bone”. This may result over the years from tiny particles of worn-out plastic or cement that may potentially migrate into the bone and cause localized damage to the bone. This condition may also result in the need for a total knee revision. That is another reason to have a yearly x-ray evaluation
Preparing For A Knee Replacement
The General Exam Prior To Surgery.
Because in most cases the patient is admitted to the hospital the morning of the surgery, the person will be scheduled for an appointment for preadmission testing several days to a few weeks before surgery usually consisting of:
- Blood work/Urine test – A complete blood count may be determined to finalize the “all clear” for surgery. Because there may be a need for blood transfusion during or after the surgery, blood tests will be needed for blood matching.
- Donating one’s own blood- If the individual chooses, they may donate their own blood prior to surgery. After this, the individual may be instructed to take iron tablets after donating the first unit of blood and to continue until admission to the hospital for the surgery.
- EKG– Provides information regarding the condition of the heart for surgery
- Chest x-ray – Provides information about the respiratory status of the individual.
- Anesthesia consult– An anesthesiologist, who is a medical doctor specializing in anesthesia, will explain what types and options of anesthesia are available for the knee surgery. Total knee replacement is either performed under a general anesthesia or under a spinal-type anesthetic. In general anesthesia, the individual is asleep during the procedure. In cases where a spinal anesthetic may be used, an injection is given into the spine numbing both legs. The individual is conscious but comfortably sedated.
- Assessment by a member of the nursing staff– The nurse will meet with the individual to explain and describe the nursing care prior to and after the surgery.
- Assessment by a social worker- This staff member will assess the needs of the patient regarding special equipment and or services the patient requires upon discharge from the hospital. The social worker can also provide the patient with a list of community resources available to meet these needs within the community and at home once discharged from the hospital.
- Assessment by a physical therapist and occupational therapist. This part of the rehabilitative team will provide preoperative education to help prepare for the surgery. The physical and occupational therapist can assist with preoperative programs to include exercises as well as arranging for special equipment that may be needed after the surgery such as walkers, canes and reaching aides.
- Other preparations
- Dental – Some individuals may be asked to have a dental check up if there has not been one recently. Dental problems that have been previously addressed before knee replacement can prevent infections that might affect the new joint.
- Eating and drinking instructions – The person undergoing surgery for total knee replacement will be given specific instructions regarding eating and drinking before surgery following guidelines from the of anesthesia department of that specific hospital.
- Current list of prescription and non-prescription medications – The physician, anesthesiologist and nursing staff will need a current list of all prescription and non-prescription medications being taken. Instructions may be given to discontinue aspirin or aspirin containing medications two weeks prior to surgery at the discretion of the surgeon.
How Is The Knee Replaced?
Once the anesthetic has been given and the patient prepared: the damaged joint surfaces are removed. An incision approximately eight inches in length is made on the front of the knee.
The damaged joint surfaces are removed from all 3 bones making up the knee joint. Sometimes, depending on the surgeon, the back of the knee cap is left intact if it is not badly affected by the arthritis. The surrounding muscles and most of the ligaments are preserved.

The lower end of the thigh bone (femur) is resurfaced with a metal cap.

The upper end of the leg bone (tibia) is replaced with a plastic and metal implant with cement and or screws.

The back of the kneecap (patella) is also resurfaced with an all-plastic implant. Highly specialized instruments are used that allow precision cutting of the bone so that the new joint fits perfectly. The type of implant used depends on surgeon’s preference and patient requirements.)
Recovery In The Hospital
The first days after total knee replacement
The first day you can expect:
- Diet may be clear liquids only
- Intravenous line in the arm for fluids and antibiotics
- Pain medication by injection, or intravenously or as tablets.
- Blood transfusion if necessary
- Activity as tolerated to include walking: (Full weight bearing if a cemented knee was used and toe touch or limited weight bearing if an uncemented knee was used).
- Breathing exercises
The second and third day you can expect:
- Exercise program initiated
The fourth day to one week you can expect:
- Progression of walking and exercises.
- Instruction on how to dress, get in and out of bed and utilize the bathroom safely.
Your Team

Postoperative care begins with a team approach of heath professionals within the hospital. Those closely involved with the postoperative total knee patient are:
The Nursing Staff
After surgery, vital signs and sensation in the lower extremities are observed and checked by the nursing staff and documented for the physician. Antibiotics are administered according to the physicians preference to reduce the risk of infection.
The surgical incision is observed closely for:
- Excessive drainage
- Proper initial healing
- The need for changing of sterile dressings
The Respiratory Therapist
The respiratory therapist is essential at this stage for:
- Instruction for coughing and deep breathing exercises to help prevent complications, such as congestion or pneumonia.
- Instruction on how use a bedside device to assist in deep breathing exercises called the Incentive Spirometer. This device along with deep breathing exercises are important to minimize the risk of lung complications after surgery by removing any excess secretions that may settle in the lungs while asleep during surgery.
The Physical Therapist
Shortly after surgery the physical therapist addresses:
- Circulation– At this point in the recovery, early stage exercises are instructed by the acute care physical therapist such as moving the ankles up and down to promote circulation and prevent clots. These exercises are often called ankle or gastrocnemius pumps.
- Range of motion– In order to aide the rehabilitation process at this stage, the physical therapist will place the operated leg in a
continuous passive motion (CPM) machine. This machine supports the leg while it slowly and gently bends and straightens the knee. This passive motion (motion performed by the machine not the patient) helps prevent stiffening and reduces postoperative scarring. It is not uncommon for this device to be started in the recovery room with the patient waking up from surgery finding their knee moving under the power of the CPM machine. - Mild muscle strengthening exercises -Once swelling has been stabilized and there is progress in the range of motion of the knee, mild strengthening and additional range of motion exercises are taught by the physical therapist to promote muscle activity and decrease muscle loss, which can occur with inactivity.
- Gait training-The physical therapist helps get you walking, beginning with short distances using crutches or a walker. This not only promotes the ability to bend the knee and strength but is also important for endurance and stamina. It is critical not to take full weight through the leg if those were the instructions given.
The Occupational Therapist
The occupational therapist is involved in evaluating and addressing how well the patient with the new knee replacement functions with activities of daily living. Issues such as how safely and independently the patient is able to dress, bathe, and care for his or herself following total knee replacement are evaluated.
Exercises Following Knee Replacement

Exercising the knee and leg muscles following surgery is extremely important to the success of the total knee replacement.
Exercises aim to quickly regain increasing motion in the knee following surgery, prevent muscle loss, which is inevitable after surgery, rebuild the muscle strength and prevent stiffness of the new knee joint.
It is important therefore, to carefully follow the rehabilitation instructions given by the physical therapists and doctors.
Standard exercises that are used for early postoperative knee replacement include:
Quadriceps Setting
This is a good beginning exercise as it not only initiates the needed muscle contraction but also is helpful in increasing extension of the knee. It is optimal for both legs as both legs will be in a weakened state postoperatively. Try to do this exercise several times every hour. However, the amount of discomfort will determine how many each individual can perform.
While lying in bed with legs straight and together and arms at the side.
- Tighten the quadriceps muscles while pushing the back of the knee downward into the bed.
- Hold this muscle contraction for four to five seconds, relax for a short period of time and repeat 10-20 times for each leg.
Terminal Knee Extension
This exercise also helps promote muscle activity and increases knee extension. This exercise is to be repeated 10-20 times.
While lying in bed place a pillow or towel rolled up into a bolster under the operated knee to position the knee joint at approximately 40 degrees from full extension.
- Tighten the quadriceps muscle and straighten the knee by lifting the heel off the bed.
- Hold this muscle contraction for 5-10 seconds, then to slowly lower the heel to the bed.
Heel Slides (Knee Flexion)
This exercise will promote muscle activity of the hamstrings as well as help increase the amount of knee flexion. The physical therapist will record the amount of flexion and extension for a daily report on the patient’s progress to be reviewed by the physician.
While lying in bed on the back, keep legs straight and together and arms at the side.
- Slide the foot of the surgical limb toward the buttock to a point where a mild stretch is felt.
- Hold this position to a count of ten then slowly returns to the starting position
Straight Leg Raising
This is another excellent exercise to promote strength to the quadriceps and the flexor muscles important in
- Bend the uninvolved leg by raising the knee and keeping the foot flat on the bed. (This will help decrease or avoid unwanted strain on the low back region).
- While keeping the involved leg straight, raise the straightened leg about six to ten inches off the bed.
- Hold this position for 5-10 seconds, then lower the leg slowly to the bed and repeat 10-20 times.
Pillow Squeeze
This is a good exercise to help strengthen the hip adductors or groin muscles.
- Place a pillow between the knees (or slightly above the knee joint line if pressure at this area is uncomfortable).
- Next squeeze the pillow and hold for a count of ten.
- Relax for a short period of time and repeat this exercise 10-20 times
Back Home After A Knee Replacement
Once you are discharged from the hospital, a nurse, physical therapist, and possibly an occupational therapist will likely see you for in-home treatment. This is to ensure your are safe in and about your home.

Home health varies from one to several visits for a safety check and review of an exercise program. In some cases, it may require up to three visits before beginning outpatient physical therapy. In other cases, the individual may be functioning adequately with his or her total knee replacement and may not require outpatient therapy.
The home exercise program is often similar to the hospital program with the progression of resistance and repetitions of strengthening exercises and increased distance and independence of ambulating.
The occupational therapist involved in the home health care of the postoperative total knee patient closely examines how safely and independently the patient is able to dress, bathe, and care for his or herself within the home environment.
Outpatient Physical Therapy

Once no longer homebound following surgery, most medical insurance will no longer provide financial coverage for home health. If a need for additional rehabilitation has been determined, outpatient physical therapy may be the next option. A new evaluation is generally conducted at the out-patient facility with new goals of rehabilitation determined at that time.
In an out-patient physical therapy clinic the physical therapist may use the following methods of treatment to help reduce persistent swelling or pain:
Thermotherapy Or Cryotherapy (use of heat or ice)
Electrical stimulation Ultrasound - Hydrotherapy (whirlpool or pool)
Progression Of Walking And Exercise
Continued use of a walker or crutches is commonplace in an outpatient setting. However, the goal is generally to progress to walking without an assistive device if possible. Depending on the surgical procedure, the physical therapist will instruct the progression of weight bearing on the surgical leg as follows:
If A Cemented Procedure Was Used:
The progression following surgery will be from using a walker, to crutches, to a cane, and concluding with independent walking with no help as tolerated.
If A Non-Cemented Procedure Was Used:
The postoperative patient may be instructed to be toe-touch only until a follow-up x-ray and/or the physician recommends to advance the amount of weight bearing (usually by the fifth or sixth week postoperatively).
Increasing the post operative patient’s endurance can be addressed through lap swimming, and using upper body exercises. The physical therapist will select a group of exercises that can be used to simulate day-to-day activities, like going up and down steps, squatting, raising up on the toes, and bending down.
Once the goals have been met in an outpatient setting regarding range of motion of the knee, strength, endurance, and ability to walk independently, the patient is ready for discharge with an independent program.
What To Expect After A Knee Replacement
Immediately after surgery there may be mild discomfort due to the operation itself. Pain medication is given to lessen any pain. However, the pain rapidly subsides and the person notices that they no longer suffer from the longstanding pain of arthritis they have endured for so many years

The healing phase will last approximately three months. During this time the mobility of the knee increases, the discomfort lessens, and ultimately the knee becomes pain free.
The new joint will again be smooth and glide easily. However, even though the newer knee may feel normal, it is not as durable as that provided by nature and so should not be abused.
Precautions And Suggestions For The First 12 Weeks Following Surgery.
Advice on Sitting
- Use a chair with arms, to assist in rising from a sit to stand position.
- Avoid sitting for periods of time longer than one hour without getting up and walking for a brief duration. If sitting for an extended period of time is unavoidable, elevate the foot to avoid excessive swelling of the lower extremity.
- Remember: If the new knee was an uncemented type, weight bearing may need to be restricted to toe-touch only for the first six weeks.
- Lifting should be restricted to loads of up to ten pounds only.
- Showering is recommended over bathing.
- Do the exercises that were recommended initially after discharge from the hospital.
- Formal supervision from a physical therapist is recommended to ensure all exercises are done properly.
Advice on getting into a car and driving
- The first step in getting into a car should be just to simply sit at the edge of the seat, followed by pulling in the legs and then pivoting to face forward.
- Driving is usually not recommended until after the first six weeks. In some cases, and under the recommendation of the surgeon, some patients may be able to return to driving a car sooner if it is equipped with an automatic transmission. and if good leg muscle control is present.
Getting Back To Your Normal Routine After A Knee Replacement
- The most significant feature following total knee replacement is relief from long-standing pain of arthritis.
- Most individuals proclaim they have dramatically improved by about six weeks, however progress continues well beyond that point.
Here are several guidelines to follow when returning to work and recreational activities:
Work
- A sedentary or less physically demanding job may be encouraged 3 to 6 weeks after surgery.
- More vigorous activities requiring prolonged walking, standing and lifting may require up to 3 months recovery.
- At times, some types of work may not be advised following total knee replacement. These may include construction, carpentry, high climbing including ladders. However, for specifics, this should be discussed at length with your surgeon.
Sports and exercise

By three months there is a dramatic improvement and the following activities are encouraged:
- General walking
- Bicycling
- Swimming
- Golfing
- Tennis
At six months to a year individuals normally do well enough to a point where they may even forget they had the surgery performed.
When To Contact Your Doctor
Contact your doctor:
- If there is unrelenting significant pain in the knee.
- If the surgical incision becomes warm, red, or appears to have an opening or drainage.
- If swelling persists/increases.
- If either of the calf regions become swollen and painful or tender to the touch.
- If you become generally warm and ill feeling.
- If chest pain or coughing develop without cause or reason.
Knee Replacement: Frequently Asked Questions
Here are some frequently asked questions related to knee replacement:
Q: How soon following total knee replacement should I be able to progress to walking independently?
A: The speed with which a person is able to discontinue the use of crutches, walker or cane varies from individual to individual. The majority of people require only a cane after six weeks, although others may need more time to progress and soon after become independent of any assistive device.
Q: How soon can one drive again after total knee replacement?
A: It is generally recommended not to drive for six weeks following total knee replacement However, if good knee control is achieved some may be able to return earlier. The surgeon will determine the appropriate time.
Q: What is a bilateral total knee replacement?
A: When both knees are replaced at the same time, the procedure is a bilateral total knee replacement. The simultaneous procedure refers to replacing both knees during one surgical event, under one anesthesia followed by a single rehabilitation period. A staged surgical procedure means that the second knee is replaced at a later period several months apart, requiring two separate hospital stays, anesthesias, and rehabilitation periods.
Q: If I have one knee replaced does this indicate I will definitely be in need of replacing the other?
A: No. Often only one knee is affected and the other completely normal. Sometimes the other knee is also affected either as severely or not as badly. The surgeon can inform you of the likelihood if the other knee will need to be replaced in the future.
Q: Will I loose a great deal of motion if I discontinue my exercise program given to me in physical therapy?
A: How high at risk you are for losing range of motion will depend how active you are with your new knee. If you are relatively active with bending and straightening you probably will not lose a significant amount if any. However, if you lead a sedentary lifestyle it is best to continue with all of the flexibility and strengthening exercises at least 3 times per week to maintain range of motion and strength.
Knee Replacement: Putting It All Together
Here is a summary of the important facts and information related to knee replacement:
- Total knee replacement (TKR) is a surgical procedure in which a painful damaged knee joint is replaced by an artificial joint.
- Osteoarthritis resulting from “wear and tear” of the knee is the most common reason individuals need to undergo knee replacement surgery.
- The decision to have a knee replacement is based on whether the painful destroyed knee is significantly affecting a persons day to day living.
- The general goal of total knee replacement is designed to provide painless and unlimited standing, sitting, walking, and other normal activities of daily living
- Improved surgical tools and procedures have led to artificial joint replacement for arthritis of the hip and knee as two of the most successful surgeries of the last century.
- The choice of surgical procedure and the type of implant depends on the surgeon’s preference and the individual patient’s requirements.
- The artificial implant is fixed to bone by either a cemented procedure or a non-cemented procedure. This will usually affect whether one can fully weight bear or only toe-touch for the first six weeks following surgery.
- Some of the most common complications following knee replacement are deep venous thrombosis (DVT), infection, stiffness and loosening of the implant.
- Postoperative care begins with a team approach of heath professionals within the hospital which include nurses, physical therapists, respiratory therapists and occupational therapists.
- Once the postoperative total knee patient has progressed to a point where they are no longer homebound from the their surgery, the patient may be a candidate for outpatient physical therapy services.
- With proper care, individuals who have undergone total knee replacement can expect a greater than ninety-five percent chance of success for at least 15 years.
Knee Replacement: Glossary
Here are definitions of medical terms related to knee replacement:
ambulating: To walk from place to place; move about
arthroplasty: An artificial joint or implant
articular cartilage: The smooth lining that covers and protects the bone ends inside a joint
avascular necrosis: Tissue death resulting from inadequate blood supply to the affected part of a bone
continuous passive motion: If a joint is moved continuously, either by another person bending it or by a machine. The continuous passive motion (CPM) machine produces continuous passive motion by slowly and gently bending and straightening the knee without the assistance of the individual.
deep venous thrombosis (DVT): formation of blood clots in the deep veins usually of the leg or pelvis
electrical stimulation: Form of treatment used in physical therapy utilizing various frequencies and wave forms of electrical current having therapeutic effects on the nervous and musculolskeletal system
electrocardiography: A procedure in which a the electrical activity of the heart is recorded
meniscus: A cartilage disk that acts as a cushion or shock absorber between the ends of bones in certain joints. In the knee the disc on the inner side of the knee is called the medial meniscus, and the disc on the outer side is called the lateral meniscus.
prosthesis: An artificial device used to replace a missing body part, such as a limb, a tooth, an eye, or a heart valve
ultrasound: Sound waves at a very high frequency of over 20,000 vibrations per second. Ultrasound has many medical applications, including raising the temperature of the soft tissues and increasing the circulation into that area.
Knee Replacement: Additional Sources Of Information
Here are some reliable sources that can provide more information on knee replacement:
American Academy of Orthopaedic Surgeons
Phone: 847/823-7186
Phone: 800/346-2267
http://www.aaos.org
American Physical Therapy Association
Phone: 800/999-APTA (2782)
http://www.apta.org
Arthritis Foundation
Phone: 404/872-7100
Phone: 800/283-7800
http://www.arthritis.org
American College of Rheumatology/Association of Rheumatology Health Professionals
Phone: 404/633-3777
Fax: 404/633-1870
http://www.rheumatology.org
National Arthritis and Musculoskeletal and Skin Diseases Information Clearinghouse (NAMSIC) National Institutes of Health
Phone: 301/495-4484
Phone: 301/ 565-2966 TTY
Phone: 301/881-2731Automated faxback system
http://www.nih.gov/niams
