In this Article
Fibroids
What Are Fibroids?
Fibroids are growths of tissue that are usually found in the wall of the uterus, or womb. They are made of a mixture of muscle tissue from the uterus and threadlike fibers of connective tissue.
Although they are called tumors, fibroids are not cancerous. Fibroids usually shrink after menopause. New fibroids do not develop before puberty or after menopause.
Fibroids are very common. They occur in 2 or 3 out of every 10 women over age 35. They occur most often in women between ages 30 and 50, although women in their 20s sometimes have them.
It is common to have more than one fibroid. Some women may have as many as a hundred. Fibroids can be as small as a pinpoint or as large as a basketball. They are usually round or oval in shape, like a ball or an egg. Their texture is firm, like an unripe peach.
Medical names for a fibroid are leiomyoma, myoma, and fibromyoma.
Fibroids can grow in different parts of the uterus. They are named according to which part of the uterus they are found
Fibroids that grow inside the wall of the uterus are called intramural fibroids. They are the most common type of fibroid.
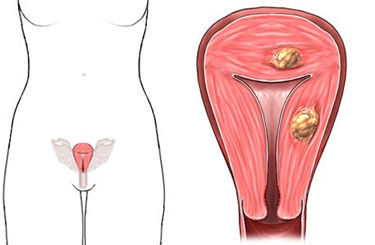
Fibroids that grow outward from the wall of the uterus into the abdominal cavity are called subserous or subserosal fibroids.

Fibroids that grow inward from the uterine wall, taking up space within the cavity of the uterus, are called submucous or submucosal fibroids.

A fibroid that is attached to the uterus by a thin stalk is called a pedunculated fibroid.

|
Facts about fibroids
|
What Causes Fibroids?
A fibroid starts as a single muscle cell in the uterus. For reasons that are not known, this cell changes into a fibroid tumor cell and starts to grow and multiply. Heredity may be a factor. It is thought that a muscle cell in the uterus may be “programmed” from birth to develop into a fibroid sometime-perhaps many years-after puberty (the start of menstrual periods).

After puberty, the ovaries produce more hormones, especially estrogen. Higher levels of these hormones may help fibroids to grow, although exactly how this might happen is not understood.
Symptoms Of Fibroids
For many women, fibroids cause no problems. More than half of women with fibroids do not know they have them until their doctor tells them so.

The most common problems caused by fibroids are:

- Heavy or long menstrual periods. Periods may last more than seven days and menstrual flow may be very heavy. Some women find they need to change sanitary napkins or tampons so often that they cannot function normally during their period. Heavy menstrual flow can sometimes lead to anemia.
- Pressure on other organs. Large fibroids may press on organs in the
pelvis .- If fibroids press on the
bladder , a woman may feel the urge to urinate frequently. She may pass only small amounts of urine and she may feel as though she has not completely emptied her bladder. - If fibroids press on the
bowel , she may feelconstipated or full after eating only a small amount of food. - If fibroids press on one or both ureters (the tubes connecting the kidneys to the bladder), they may partially block the flow of urine. A woman may not be aware of this because it often isn’t painful. Over time, however, this kind of blockage can lead to kidney infections or other serious kidney damage.
- If fibroids press on the
- Pain in the pelvis. The pressure of large fibroids on other organs may cause pain in the pelvis. Sometimes, if fibroids do not get the blood flow they need to sustain themselves, they degenerate or die. This may cause severe pain lasting for days or weeks. Pain may also occur if the stalk of a fibroid twists, cutting off blood supply to the fibroid. Rarely, a fibroid may become infected and cause pain.

|
Need To Know Problems like those caused by fibroids can also have other causes. It is important to rule out these other possible causes of any problems a woman is having. For example, an imbalance of hormones may cause heavy periods. A bladder infection can cause a frequent need to urinate. |
Who Is Likely To Get Fibroids?
Fibroids can occur in any woman of reproductive age. African American women are three times as likely as Caucasian women to have fibroids. It is not known how common fibroids are in women of other races and ethnic backgrounds.
Do I Have Fibroids?
Many women learn they have fibroids when their doctor performs a routine pelvic exam. A uterus that is enlarged or irregular in shape is a sign that a woman may have fibroids. Certain tests help the doctor to be sure of the diagnosis.

- Ultrasound. During this test, sound waves too high-pitched to be heard travel from a handheld instrument that is placed gently on the abdomen or in the
vagina . The sound waves “bounce” off of internal organs and return to the instrument. This creates a picture of the internal organs that can be seen on a screen. If there are fibroids in the uterus, they can be seen in the picture. The doctor can measure the fibroids and can also see if anything else is causing enlargement of the uterus.An ultrasound exam usually takes 15 to 30 minutes. The test does not use X-rays and has no known risks. It is safe to do an ultrasound test on a woman who is pregnant. (The handheld instrument is placed on the abdomen of a pregnant woman.) A woman may feel some discomfort because she needs to have a full
bladder during the test. - Magnetic resonance imaging (MRI). This test uses powerful magnets to create a picture of the internal organs. It does not use X-rays, and it is not necessary to have a full bladder. The test takes 30 to 45 minutes. MRI tests are not done routinely because they are much more expensive than ultrasound tests. It is safe to do an MRI test on a woman who is pregnant but it is usually avoided. To learn more about MRI scans GO TO MRI
If the doctor suspects fibroids, why might he or she order an MRI test?
The doctor may decide to order an MRI:
- if the
ovaries are difficult to see during the ultrasound test - if the doctor wants to see the structure of the fibroids in more detail
- if the
- CT scan. If MRI is unavailable, the doctor may request a CT scan of the
pelvis . CT stands for computerized tomography. A CT scan uses X-rays. It is more expensive than an ultrasound test and may not provide any more information than the ultrasound test did. For these reasons, it is rare for a doctor to order a CT scan for suspected fibroids. A woman cannot have a CT scan if she is pregnant. - Hysteroscopy. This test allows the doctor to look directly into the cavity of the uterus. The doctor may decide to do a hysteroscopy if a woman is having heavy bleeding, is having trouble becoming pregnant, or if fibroids are suspected of causing other
fertility problems (for example, a miscarriage). A woman cannot have a hysteroscopy if she is pregnant.What happens during a hysteroscopy?
A thin telescope called a hysteroscope is gently inserted through the
cervix and into the uterus. Enlarging the opening of the cervix to insert the hysteroscope can cause cramping and mild bleeding. Doctors generally advise women to take a mild pain medication before and, if necessary, after the procedure.A hysteroscopy may be done in a doctor’s office (with local or no anesthesia) or in an operating room (with local or general anesthesia).
- Uterine X-ray. This test is another option for diagnosing fibroids in women who are having bleeding or fertility problems. A woman cannot have a uterine X-ray if she is pregnant.
What happens during a uterine X-ray?
An instrument is gently inserted into the opening of the cervix. Dye is injected, filling the uterus. The doctor can see the shape of the uterine cavity and can take X-ray pictures of the uterus and
fallopian tubes . The doctor can see if the tubes are blocked because the dye will not pass through them.This test may cause cramping. Doctors generally advise women to take a mild pain medication an hour or so before the test, which is done in a radiology suite (with local or no anesthesia). The dye is harmless (unless a woman has an allergy to iodine or shellfish) and it is quickly removed from the body.
Medical names for this test are hysterosalpingogram (or HSG) and uterotubogram.
- Endometrial biopsy. In this test, a small piece of the lining of the uterus (the endometrium) is removed and examined under a microscope. The doctor may suggest an endometrial biopsy if a woman is having heavy or lengthy periods. The purpose of the test is to rule out other causes for the bleeding, such as infection, a
polyp , or cancer.What happens during an endometrial biopsy?
A thin tube is gently passed through the cervix to obtain a piece of tissue from the lining of the uterus. This takes only a few minutes. The test may cause cramping. It can usually be performed in a doctor’s office with local or no
anesthesia . - Dilatation and curettage (D&C). This test is another way to obtain a small (or somewhat larger) piece of the lining of the uterus. It might be done instead of an endometrial biopsy if more tissue is needed or if an endometrial biopsy cannot be done.
What happens during a D&C?
The opening of the cervix is gently enlarged (dilated) by inserting metal probes of increasing thickness. Then, a scraping instrument is passed through the enlarged opening of the cervix to obtain a piece of tissue from the lining of the uterus. A D&C is performed in an operating room. Local or general anesthesia may be used.
The doctor also needs to rule out other problems that can cause the same symptoms as fibroids. For example, an imbalance of hormones may cause heavy periods. A bladder infection can cause a frequent need to urinate.
Can Fibroids Lead To Cancer?
In most women, fibroids do not lead to cancer. Rarely, however, fibroids can turn into a cancer called a leiomyosarcoma. This happens to an estimated 1 in 1,000 women who have fibroids. Some cancerous tumors may develop directly from normal tissue in the uterus. The average age of women with leiomyosarcoma is 55.
Warning signs of cancer may include:
- rapid growth of the fibroids or the uterus
- vaginal bleeding after a woman has passed
menopause .
If a woman has either of these problems, she should see a doctor right away.
Do Fibroids Affect Pregnancy?
Most women with fibroids have no more trouble becoming pregnant than women who do not have fibroids, and their risk of a bad pregnancy outcome is no higher.
About 1 in every 15 women with infertility has fibroids, but the fibroids are usually innocent bystanders: They cause only 2% to 3% of cases of infertility. Fibroids that block one or both of the fallopian tubes may prevent sperm from fertilizing an egg. Fibroids that fill the uterine cavity may block implantation of a newly fertilized egg.
Fibroids-especially those located in the cavity of the uterus-may increase the chance of a miscarriage or may cause a woman to go into labor before her due date (premature labor). Fibroids may also increase the chance that the baby is not positioned to come out headfirst. This can increase the need for cesarean section. Rarely, fibroids can cause complications of pregnancy called placental abruption and postpartum hemorrhage.
What Is Placental Abruption?
After childbirth, the afterbirth (
In addition to causing vaginal bleeding and pain, placental abruption can cut off the baby’s supply of nutrients and blood. In severe cases, this can threaten the baby’s life.
What Is Postpartum Hemorrhage?
Normally, the afterbirth (placenta) separates from the uterus after childbirth. When this happens, the muscle in the uterus usually squeezes the uterus to help stop bleeding. If a fibroid is present, the squeezing of the muscle in the uterus may be less effective and the woman may have more bleeding. Rarely, the blood loss may be significant and the woman may need medications, surgery, and/or a
Some fibroids grow during pregnancy, but some remain the same size and others shrink.
Do Fibroids Need To Be Treated?
If fibroids are not causing problems, regular checkups may be the only management they need. This is called watchful waiting. The doctor examines a woman two or three times a year to see if the fibroids are growing and if they are beginning to cause problems. If the doctor cannot feel the woman’s ovaries during a pelvic exam, ultrasound should be performed once a year.
Problems like those caused by fibroids can also have other causes. It is important to rule out these other possible causes of any problems a woman is having. For example, an imbalance of hormones may cause heavy periods. A bladder infection can cause a frequent need to urinate.
How Are Fibroids Treated?
The treatment offered for fibroids will depend on whether or not the fibroids are causing any problems.
- If fibroids are not causing problems, they may need no treatment apart from regular medical checkups. This is called watchful waiting. The doctor examines a woman two or three times a year to see if the fibroids are growing and if they are beginning to cause problems. If the doctor cannot feel the woman’s
ovaries during a pelvic exam, ultrasound should be performed once a year. - Surgery is the standard treatment for fibroids that are causing pain, heavy or lengthy menstrual bleeding, or other problems. The two kinds of surgery most commonly performed arehysterectomy and myomectomy.
- The two kinds of surgery most commonly performed arehysterectomy and myomectomy (see below).
- There are quite a few newer treatment options that offer alternatives to hysterectomy (click here to go to this section)
- There is also a role for special medications in the treatment of fibroids, either to shrink the fibroid to allow for a simpler type of surgery, or for women just before
menopause (fibroids shrink naturally during menopause). See Treatment with Medication

Hysterectomy
Hysterectomy is the surgical removal of the
Hysterectomy is often considered when the uterus reaches the size it would be at 12 weeks of pregnancy. In the past, many doctors recommended a hysterectomy because they feared that such large fibroids could hide the presence of cancer of the uterus.
Now, however, tests such as ultrasound and MRI can be used to see whether a fibroid is growing rapidly (a sign of cancer). Increased use of these tests has reduced the number of hysterectomies performed for fibroids.
How is a hysterectomy performed?
A hysterectomy is usually performed through an
What is a vaginal hysterectomy?
Sometimes, for smaller fibroids, the uterus can be removed through the
Occasionally a surgeon will perform a vaginal hysterectomy assisted by laparoscopy. This is called a laparoscopic-assisted vaginal hysterectomy.
What are the risks of a hysterectomy?
Like all operations, a hysterectomy has risks. These include:
- infection requiring treatment with antibiotics (1 in 5 women)
- internal bleeding (hemorrhage) requiring a
blood transfusion (1 in 15) - injury to other pelvic organs such as the
bladder ,bowel , or ureters (less than 1 in 100) - death (1 in 2,000)
What happens after a hysterectomy?
A woman usually stays in the hospital for two to five days after an abdominal hysterectomy. Full recovery usually takes about six weeks. Women are generally advised to avoid driving and heavy lifting for two to four weeks after surgery. Light exercise may begin after four weeks. Vigorous exercise and sexual intercourse should be avoided for six weeks after surgery.
After a vaginal hysterectomy, a woman may stay in the hospital for two to four days and recover fully in three to four weeks. She can expect to have a light-brown vaginal discharge for about six weeks after surgery. Women are usually advised not to have sexual intercourse for six weeks after a vaginal hysterectomy. Intercourse should only resume after the surgeon has examined her vagina to assure that it has completely healed.
Myomectomy
Myomectomy is the removal of fibroids without removing the uterus. This operation preserves a woman’s ability to bear children. However, a successful pregnancy is not guaranteed. Only 4 or 5 out of 10 women become pregnant and give birth after a myomectomy.
Heavy bleeding can occur when the fibroids are removed. A woman is more likely to need a blood transfusion after a myomectomy than after a hysterectomy. She is also at higher risk for problems such as infection and blood clots in the legs.
Fibroids may grow back after a myomectomy, and another operation may be needed later to remove them. The risk of regrowth is related to the number, not the size, of fibroids removed. If more than three fibroids are removed, the risk of regrowth is about 50-50.
How is a myomectomy performed?
Like a hysterectomy, a myomectomy is usually performed through an incision in the abdomen. The risks and recovery time are about the same as for a hysterectomy. Sometimes a myomectomy can be performed with the assistance of a laparoscope or hysteroscope.
Why can it be difficult to become pregnant after a myomectomy?
When the uterus heals after surgery, scarring can occur. Scars may cover the ovaries or block one or both of the
A woman who becomes pregnant after a myomectomy may be advised by her doctor to have a
Fibroids: Newer Treatment Options
Several new procedures offer alternatives to hysterectomy or myomectomy, especially for the removal of smaller fibroids. An advantage of these new procedures is that they do not involve abdominal surgery. They may be performed on an outpatient basis, or they may require only an overnight hospital stay. Recovery time is usually quicker, too. However, because these procedures are new, many doctors have little experience with them.
- Hysteroscopic resection. This procedure uses a hysteroscope, a thin telescope that is inserted through the cervix. It enables the surgeon to see inside the uterus. The surgeon may then remove the fibroids with a laser or an electrical knife, wire, or probe. No incision is made. The procedure may be done with local or general anesthesia. The woman may stay overnight in the hospital or be treated as an outpatient. Full recovery takes a week or two.
- Embolization. This procedure shrinks fibroids by cutting off their blood supply. Guided by an X-ray image, the doctor threads a small
catheter (a thin flexible tube) through a tiny incision in thegroin into the main arteries that supply blood to the uterus. He or she then injects particles of inert plastic through the catheter to block these blood vessels. The uterus itself is not damaged because smaller arteries continue to supply the nutrients and oxygen it needs.The procedure takes about an hour. It may be performed with local or general anesthesia. The woman must lie flat on her back for six hours afterward to stop bleeding from the incision in the groin. Cramps in the
pelvis are common, and the doctor usually prescribes a pain medication for them. Some women may have a fever for a couple of days after the procedure. Some women stay overnight in the hospital, while others go home the same day. Full recovery takes about a week.Embolization has been used to treat fibroids in the United States for only a few years. Typically, the procedure shrinks fibroids to about half their previous size. The fibroids also become softer and press less on other pelvic organs. It is not known, however, whether the fibroids eventually grow back.
- Laparoscopic surgery . Some procedures can be performed using a laparoscope, a pencil-thin surgical telescope similar to a hysteroscope. The surgeon inserts the laparoscope and tiny surgical instruments through one or more small incision in the abdomen.
If the fibroids are small and easy to reach, the surgeon makes an incision in the uterus and removes them. This is called a laparoscopic myomectomy. It may require an overnight hospital stay.
When the fibroids are larger or harder to reach, the surgeon may use a laser or an electric needle to destroy or shrink them. This procedure is known as laparoscopic myolysis. Women who have this procedure done can often go home the same day.
Full recovery from laparoscopic surgery generally takes less than 7 days.
Can Fibroids Be Treated With Medication?
Doctors may prescribe drugs called gonadotropin-releasing hormone agonists (GnRH agonists) to treat fibroids. Most fibroids shrink by one-third to one-half of their original size after two to three months of treatment with these drugs. Smaller fibroids may cause fewer problems and they are often easier to remove surgically.
Women should not take GnRH agonists for more than six months. After that, the drugs can cause rapid bone loss, leading to osteoporosis. Fibroids generally start to grow again once drug treatment stops. Most women stop having menstrual periods while they are taking GnRH agonists.
What Are GnRH Agonists?
GnRH agonists are drugs that are chemically similar to gonadotropin-releasing hormone (GnRH). This hormone is produced by the hypothalamus, a region in the brain.
GnRH stimulates the release of other hormones from the pituitary gland, a pea-sized gland at the base of the brain. These other hormones areluteinizing hormone and follicle-stimulating hormone. They, in turn, stimulate the ovaries to produce estrogen. GnRH agonists block that process, shutting down estrogen production. Deprived of estrogen, fibroids shrink.
GnRH agonists are approved by the U.S. Food and Drug Administration to treat
- Lupron (leuprolide)
- Synarel (nafarelin)
- Zoladex (goserelin)
How Are GnRH Agonists Used To Treat Fibroids?
Doctors may use these drugs in more than one way to treat fibroids.
- If a woman is close to
menopause , a doctor may prescribe GnRH agonists for a few months to shrink her fibroids. After menopause, fibroids shrink naturally because estrogen levels in the body decline. - A doctor may prescribe GnRH to shrink fibroids before a woman has surgery. Smaller fibroids may make it possible for a woman to have a vaginal hysterectomy instead of an abdominal one. She may also be able to have laparoscopic surgery, which requires a shorter hospital stay and has a faster recovery time.
What Side Effects Do GnRH Agonists Have?
By blocking estrogen production, GnRH agonists mimic a process that occurs naturally at menopause. The side effects of these drugs are similar to the problems many women have when they go through menopause.
The most common problem (experienced by about 9 out of 10 women) is hot flashes-episodes of suddenly feeling very warm in the face or upper body. During a hot flash, a woman may blush, perspire, or feel her pulse racing. A cold chill may follow the hot flash. Hot flashes are caused by declining or unstable estrogen levels in the body.
Other less common side effects of GnRH agonists include:
- vaginal dryness
- irregular vaginal bleeding
- headaches
- thinning of the hair
- pain in the bones, joints, and muscles
- sleep problems
- mood changes
- loss of sex drive
Doctors may also prescribe synthetic hormones to reduce heavy bleeding caused by fibroids. Progestogen is a synthetic version of the female hormone
Some doctors may prescribe a GnRH agonist in combination with a low dose of estrogen or progestogen. Low doses of these hormones may reduce the side effects of GnRH agonists, which may allow women to be treated safely with these drugs for a longer time.
Choosing The Best Treatment For Fibroids
No treatment for fibroids is best for all women who have this problem. Every woman should discuss the treatment options with her doctor. The treatment that is best for any individual woman will depend on a variety of factors.
- Are the fibroids causing problems? Fibroids that are not causing problems may need no treatment at all. A woman should be checked by her doctor every few months to see if the fibroids are growing. If the fibroids begin to cause problems, it’s time to consider treatment options.
- What problems are the fibroids causing? The best treatment choice may be different if fibroids are causing severe pain than if a woman’s major problem is heavy bleeding. Treatment that shrinks fibroids (embolization, treatment with a GnRH agonist drug) often relieves pain. Heavy bleeding may be treated by combination therapy with a GnRH agonist and a low-dose
hormone . - Do you want to have more children? Fibroids in the
uterus usually do not prevent a woman from becoming pregnant. However, a woman cannot become pregnant or carry a baby after having a hysterectomy (removal of the uterus). A myomectomy preserves the uterus but may make it more difficult to become pregnant. - Do you want to avoid having major surgery? A hysterectomy is major surgery, requiring two to five days in the hospital and about six weeks to recover fully. Some women-and some doctors-feel that a hysterectomy is undesirable for a problem such as fibroids that is not life-threatening. However, a myomectomy is also major surgery, requiring about the same length of time in the hospital and about the same recovery time as a hysterectomy.
Women who want to avoid major surgery may wish to consult a doctor who has experience in one or more of the new procedures that in some cases offer alternatives to hysterectomy or myomectomy.
- Are you close to
menopause ? Fibroids shrink naturally after menopause whenestrogen levels in the body decline. If a woman who is close to menopause has pain caused by fibroids, a doctor may prescribe GnRH agonists. Treatment with these drugs for a few months will shrink her fibroids, which should relieve her pain until the fibroids begin to shrink naturally after menopause.
Fibroids: Frequently Asked Questions
Here are some frequently asked questions related to fibroids.
Q: Can I take birth control pills if I have fibroids?
A: Birth control pills contain
Q: If I’m past
A: Many doctors recommend that women take low doses of the hormone estrogen, or a combination of estrogen and
Q: I’m 45. My
A: If your fibroids are not causing problems, such as heavy bleeding, pelvic pain, and frequent urination, you and your doctor may consider watchful waiting. This means you would have pelvic examinations two or three times a year to see if the fibroids are growing or are beginning to cause problems. If your fibroids are causing problems, you may want to ask your doctor about treating them with medication. Taking GnRH agonist drugs for two to three months could shrink your fibroids by one-third or one-half of their present size. This may relieve problems such as pain or heavy bleeding. These drugs will stop you from having a menstrual period and they have side effects similar to those of menopause. Your fibroids will probably grow back after you stop taking the medication. However, when your fibroids have shrunk you may be a candidate for a less invasive procedure to remove them, such as hysteroscopic resection, embolization, or laparoscopic surgery.
Fibroids: Putting It All Together
Here is a summary of the important facts and information related to fibroids.
- Fibroids are growths of tissue that are usually found in the wall of the
uterus . They can be as small as a pinpoint or as large as a basketball. - Although they are called tumors, fibroids are not cancerous.
- More than half of women with fibroids do not know they have them until their doctor tells them so.
- The most common problems caused by fibroids are heavy or long menstrual periods, pressure on other organs, and pain in the
pelvis . For many women, however, fibroids cause no problems. - In most women, fibroids do not lead to cancer.
- If fibroids are not causing problems, regular checkups may be the only management they need.
- Surgery is the standard treatment for fibroids that are causing problems. The two kinds of surgery most commonly performed are hysterectomy (removal of the uterus) or myomectomy (removal of fibroids without removing the uterus).
- Several new procedures offer alternatives to hysterectomy or myomectomy, especially for the removal of smaller fibroids. In some cases, fibroids may also be treated with medication.
- Fibroids usually shrink after
menopause . - New fibroids do not develop before puberty or after menopause.
Fibroids: Glossary
Here are definitions of medical terms related to fibroids.
Anemia: Too few red blood cells in the blood. This results in too little oxygen getting to tissues and organs. Symptoms are feeling easily or always tired, lack of skin color, and getting frequent infections. Sometimes referred to as “low blood count.”
Anesthesia: Loss of feeling or sensation in all or part of the body. Usually used to mean loss of sensation of pain, which is achieved by giving drugs before surgery. General anesthesia is total unconsciousness. Local anesthesia is loss of sensation in part of the body; it is used for minor surgery.
Artery: A blood vessel that carries blood away from the heart.
Bladder: Organ in the pelvic region that stores urine.
Blood transfusion: The process of injecting additional blood into a sick person. Usually the blood is donated by a healthy person. Sometimes a person will have some of their own blood drawn and stored before having surgery and re-injected after surgery. This is called an autologous blood transfusion.
Bowel: A general term for the small and large intestines, the organs that digest and eliminate food.
Catheter: A flexible tube that is inserted into an opening in the body. It may be used to drain fluids from the body or to insert fluids into the body.
Cervix: The neck of the uterus, which connects the uterus with the vagina.
Cesarean section: Surgery to deliver a baby by cutting open the abdomen and uterus. Recommended when a vaginal delivery is considered dangerous to the baby and/or the mother.
Constipated: Suffering from difficult, painful, or infrequent movement of the bowels.
Diagnosis: Identifying a disease based on its signs and symptoms.
Endometriosis: A disease in which tissue similar to the lining of the uterus (endometrium) is found in other organs in the pelvic region. Symptoms are pain in the pelvis and painful menstrual bleeding.
Estrogen: A hormone that promotes the growth and development of breasts, female sex organs, other female sexual characteristics.
Fallopian tubes: Tubes through which eggs travel from the ovaries to the uterus each month during ovulation.
Fertility: The ability to become pregnant and give birth to a child.
Groin: The area of the body where the thigh meets the abdomen.
Hemorrhage: Heavy or uncontrollable bleeding.
Hormone: A substance produced by the body that stimulates activity by organs or tissues elsewhere in the body. Estrogen and progesterone are female sex hormones.
Incision: A cut made in the body to perform surgery.
Laser: A device that produces a thin, high-energy light beam. Used in surgery to operate on a small area of the body without damaging surrounding tissue.
Menopause: The period in a woman’s life when ovulation and menstrual periods stop and she is no longer able to bear children. Levels of the sex hormones estrogen and progesterone decline at menopause. This can cause symptoms such as hot flashes and vaginal dryness.
Osteoporosis: A condition in which the bones weaken due to loss of calcium and are prone to fracture. A common condition in older women.
Ovaries: Female reproductive organs located on either side of the uterus. The ovaries produce eggs and the hormones estrogen and progesterone.
Ovulation: The monthly process in which an egg, released from the ovaries, travels through the fallopian tubes to the uterus.
Pelvis: A basin-shaped cavity in the lower abdomen, containing the bladder, bowel, and reproductive organs.
Placenta: A special lining that grows within the uterus during pregnancy to nourish the developing fetus. Sometimes called the afterbirth because it is expelled from the uterus a few hours after childbirth.
Polyp: A growth in a bodily organ that is lined by a moist membrane. Polyps are usually benign (not cancerous).
Postpartum: The period of time immediately after childbirth.
Progesterone: A hormone that promotes the growth and development of breasts, female sex organs, other female sexual characteristics.
Side effect: An unwanted effect produced by a medication or other medical treatment.
Tranquilizer: A medication that produces a calming effect, relieving tension and anxiety.
Tumor: An abnormal mass of tissue that results from excessive cell division. A tumor may be benign (not cancerous) or malignant (cancerous). A fibroid tumor is benign
Uterus: The female reproductive organ in which a fetus grows during pregnancy. Also called the womb.
Vagina: The female organ of sexual intercourse. Also the passage through which a baby is delivered in normal childbirth.
Fibroids: Additional Sources Of Information
Here are some reliable sources that can provide more information on fibroids.
American College of Obstetricians and Gynecologists
409 12th St., SW
Washington, D.C.20024-2188
Phone: 202-638-5577
Online: http://www.acog.com
ACOG is a professional association for obstetricians and gynecologists. Its resource center offers information for health care consumers on obstetric and gynecological health conditions.

