In this Article
AIDS And Women
What Is AIDS?
AIDS stands for Acquired imunodeficiency (or immune deficiency) Syndrome. It results from infection with a virus called HIV, which stands for human immunodeficiency virus. This virus infects key cells in the human body called CD4-positive (CD4+) T cells. These cells are part of the body’s immune system, which fights infections and various cancers.
When HIV invades the body’s CD4+ T cells, the damaged immune system loses its ability to defend against diseases caused by bacteria, viruses, and other microscopic organisms. A substantial decline in CD4+ T cells also leaves the body vulnerable to certain cancers.
There is no cure for AIDS, but medical treatments can slow down the rate at which HIV weakens the immune system. As with other diseases, early detection offers more options for treatment and preventing complications.
AIDS affects women differently than it does men, and it presents unique issues related to sexuality, childbearing, and side effects of treatments.
What Is The Difference Between HIV And AIDS?
The term AIDS refers to an advanced stage of HIV infection, when the immune system has sustained substantial damage. Not everyone who has HIV infection develops AIDS.
When HIV progresses to AIDS, however, it has proved to be a universally fatal illness. Few people survive five years from the time they are diagnosed with AIDS, although this is increasing with improvements in treatment techniques.
Experts estimate that about half the people with HIV will develop AIDS within 10 years after becoming infected. This time varies greatly from person to person, however, and can depend on many factors, including a person’s health status and health-related behaviors.
People are said to have AIDS when they have certain signs or symptoms specified in guidelines formulated by the U.S. Centers for Disease Control and Prevention (CDC).
The CDC’s definition of
- All HIV-infected people with fewer than 200 CD4+ T cells per cubic millimeter of blood (compared with CD4+ T cell counts of about 1,000 for healthy people)
- People with HIV infection who have at least one of more than two dozen AIDS-associated conditions that are the result of HIV’s attack on the immune system
AIDS-associated conditions include:
Opportunistic infections by bacteria, fungi, and viruses. Opportunistic infections are infections that are rarely seen in healthy people but occur when a person’s immune system is weakened.- The development of certain cancers (including cervical cancer and lymphomas)
- Certain autoimmune disorders Autoimmune disorders are illnesses that result when the immune system attacks an individual’s own tissues or cells.

Most AIDS-associated conditions are rarely serious in healthy individuals. In people with AIDS, however, these infections are often severe and sometimes fatal because the immune system is so damaged by HIV that the body cannot fight them off.
The History Of AIDS
The symptoms of AIDS were first recognized in the early 1980s:
- In 1981, a rare lung infection called Pneumosystis cariniipneumonia began to appear in
homosexual men living in Los Angeles and New York. - At the same time, cases of a rare tumor called
Kaposi’s sarcoma were also reported in young homosexual men. These tumors had been previously known to affect elderly men, particularly in parts of Africa. New appearances of the tumors were more aggressive in the young men and appeared on parts of the body other than the skin. - Other infections associated with weakened immune defenses were also reported in the early 1980s.
Groups most frequently reporting these infections in the early 1980s were homosexuals, intravenous drug users, and people with hemophilia, a blood disorder that requires frequent transfusions. Blood and sexual transmission were therefore suspected as the sources for the spread of the infections.
In 1984, the responsible virus was identified and given a name. In 1986, it was renamed the human immunodeficiency virus (HIV).
Need To Know:
Because many of the first cases of AIDS in the United States occurred in homosexual men and intravenous drug users, some people mistakenly believe that other groups of people are not at risk for HIV infection. However, anyone is capable of becoming HIV-infected, regardless of gender, age, or sexual orientation.
Facts About AIDS
- As of the year 2000, nearly one million people in the U.S. were confirmed to be HIV-positive.
- The Centers for Disease Control and Prevention reports that 2.2 million Americans now carry the HIV virus but do not yet have symptoms.
- About one out of every three people with HIV infection in the U.S. is a woman.
- AIDS is a leading cause of death for American men and women between the ages of 25 and 44.
- Since 1992, AIDS has been the fourth leading cause of death among U.S. women between the ages of 25 and 44.
- Through June 2000, 438,795 people in the U.S. had died from AIDS (374,422 men and 64,373 women).
- By the end of 2000, 36.1 million people worldwide were living with HIV/AIDS, with the vast majority living in developing countries.
- Through 2000, 21.8 million people worldwide have died from AIDS.
- Between 1991 and 1996, there were more new cases of AIDS among people older than 50 than those between ages 13 and 49. Today, 11% of all new cases of AIDS in the U.S. are now in people over the age of 50.
- The
HIV carrier rate in the U.S. is now 1 carrier for every 100 to 200 people. - Teenage and young adult women currently make up half of all new HIV infections reported in people 13 to 24 years old.
What Causes AIDS?
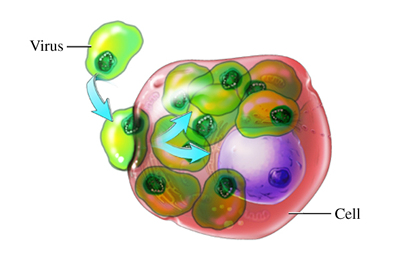
HIV is a type of virus called a retrovirus. Like all viruses, it must invade the cells of other organisms to survive and reproduce. HIV multiplies in the human immune system’s CD4+ T cells and kills vast numbers of the cells it infects. The result is disease symptoms.
Nice To Know:
There are two forms of HIV:
- HIV-1 is the more common and more potent form. This form of HIV has spread throughout the world.
- HIV-2, which is less potent that HIV-1, is found predominantly in West Africa. It is also more closely related to two HIV-like viruses found in monkeys.
There also are different strains of the virus, which makes it difficult to find one single treatment.
About The Immune System
Our bodies use a natural defense system to protect us from bacteria, fungi, viruses, and other microscopic invaders. This system includes general, nonspecific defenses as well as weapons custom-designed against specific health threats:
- Innate, or nonspecific,
immunity is the first line of defense. Our skin, tears, mucus, and saliva, as well as the swelling that occurs after an infection or injury, contain types of immune cells and chemicals that attack disease-causing agents attempting to invade the body. - Adaptive, or specific, immunity uses specialized cells and proteins called
antibodies to attack invaders that get past the first line of defense. These weapons target specific proteins called antigens, found on the surface of the invading organism. Theimmune system can quickly rally these custom-tailored defenses if this particular invader attacks again.
There are two types of adaptive immune responses:
- The humoral immune response involves the action of specialized antibody-producing white blood cells. The antibodies (proteins produced by the immune system to fight infectious agents such as viruses), which circulate in the blood and other body fluids, can recognize specific antigens (substances that stimulate the production of antibodies). They latch onto the viruses, bacteria, toxins, and other substances that bear these antigens, targeting them for destruction.
- The cell-mediated immune response involves the action of another group of specialized white blood cells that direct and regulate the body’s immune responses or directly attack cells that are infected or cancerous.
How Do White Blood Cells Help Fight Disease?
White blood cells, particularly
- Macrophages contribute to both nonspecific and specific immune responses. These versatile cells act as scavengers, engulfing and digesting microbes and other foreign material in a cell-eating process called
phagocytosis . They also, upon encountering an invading organism, release chemical messengers that alert other cells of the immune system and summonT lymphocytes to the scene. B lymphocytes , or B cells, serve as the body’s antibody factories. Each antibody is targeted to recognize and bind to anantigen from a specific invader. When antibodies circulating through blood and body fluids encounter this invader, they mark it for destruction.- T lymphocytes, or T cells, are part of the cellular immune response. Some T cells, like CD4+ T cells (also called “helper” T cells), direct and regulate the body’s immune responses. Others are killer cells that attack cells that are infected or cancerous.
How Does HIV Infection Become Established In The Body?
Researchers have found evidence that immune-system cells called dendritic cells may begin the process of infection. After exposure, these special cells may bind to and carry the virus from the site of infection to the lymph nodes, where other immune system cells become infected.
HIV targets cells in the immune system that display a protein called
Nice To Know:
When HIV encounters a CD4+ cell, a protein called gp120 that protrudes from HIV’s surface recognizes the CD4 protein and binds tightly to it. Another viral protein, p24, forms a casing that surrounds HIV’s genetic material.
HIV’s genetic material contains the information needed by the virus to infect cells, produce new copies of virus, or cause disease. For example, these genes encode enzymes that HIV requires to reproduce itself. Those enzymes are
How Do Women Get AIDS?
HIV infection is spread in three ways:
However, there is much misunderstanding about the ways in which HIV infection is not spread.
About one out of every three people in the U.S. infected with HIV, the virus that can lead to AIDS, is a woman. In the U.S., most HIV-infected women become infected during sex with an HIV-infected man or while using HIV-contaminated needles and syringes for injection drugs.
Nice To Know:
According to a 1999 survey, of the women who were diagnosed with HIV infection in the previous year:
- 13% were infected through injection drug use.
- 36% were infected through having sex with men, including injecting drug users,
bisexual orheterosexual men, or men with hemophilia. - Less than 1% were infected from receiving blood transfusions or treatment with blood components or tissues containing HIV.
- In about half of these women, the cause of infection was not reported or identified.
In some areas of the world, including countries in Africa and Asia, most women are infected through sex with heterosexual men.
Sexual Intercourse
HIV is spread most commonly by sexual contact with an infected partner. The virus can enter the body through the lining of the vagina, penis, rectum, or mouth during sexual relations.
Sexual activities that can result in HIV infection include:
- Sexual intercourse
- Anal sex (heterosexual or
homosexual ) - Oral sex (heterosexual or homosexual)
Need To Know:
Q: Can HIV be spread through kissing?
A: Although studies have found tiny amounts of HIV in the saliva of some people with HIV, researchers have found no evidence that HIV is spread to other people through kissing. However, the CDC recommends against “French” or open-mouthed kissing because of the possibility of contact with blood if the people kissing have any cuts or sores in the mouth.
Direct Contact With Infected Blood
HIV can be spread through direct contact with infected blood:

- Through injected drugs. HIV frequently is spread among users of illegal drugs that are injected. This happens when needles or syringes contaminated with minute quantities of blood of someone infected with the virus are shared.
- In a health-care setting. Transmission from patient to health-care worker or vice-versa – via accidental sticks with contaminated needles or other medical instruments – can occur, but this is rare.
- Through a blood
transfusion . Prior to the screening of blood for evidence of HIV infection and before the introduction in 1985 of heat-treating techniques to destroy HIV in blood products, HIV was transmitted through transfusions of contaminated blood or blood components. Today, because of blood screening and heat treatment, the risk of acquiring HIV from such transfusions is extremely small.
From An Infected Mother To Her Unborn Child
Women can transmit HIV to their fetuses during pregnancy or birth. Approximately one-quarter to one-third of all untreated pregnant women infected with
A pregnant woman can greatly reduce the risk of infecting her baby if she takes the anti-HIV drug
HIV also can be spread to babies through the breast milk of mothers infected with the virus.
- Women who live in countries where safe alternatives to breast-feeding are readily available and affordable can eliminate the risk of transmitting the virus through breast milk by bottle-feeding their babies.
- In developing countries, however, where such safe alternatives are not readily available or economically feasible, breast-feeding may offer benefits that outweigh the risk of HIV transmission.
How Is HIV Infection Not Spread?
Research indicates that HIV is NOT transmitted by casual contact such as:
- Touching or hugging
- Sharing household items such as utensils, towels, and bedding
- Contact with sweat or tears
- Sharing facilities such as swimming pools, saunas, hot tubs, or toilets with HIV-infected people
- Coughs or sneezes
In short, studies indicate that HIV transmission requires intimate contact with infected blood or body fluids (vaginal secretions, semen, pre-ejaculation fluid, and breast milk). Activities that don’t involve the possibility of such contact are regarded as posing no risk of infection.
Need To Know:
Q: Is it safe to share a household with an HIV-infected person?
A: Studies of families of HIV-infected people have found that HIV is not spread through sharing utensils, towels, bedding, or toilet facilities. Behaviors that increase the likelihood of contact with blood from an HIV-infected person, such as sharing a razor or toothbrush, should be avoided.
Teenage and Young Adult Women
Teenage and young adult women now make up half of all new HIV infections reported in people 13 to 24 years old. Among U.S. adolescent AIDS cases, the number of females represented tripled from 1987 to 1994.
Many American teenagers are engaging in behaviors that may put them at risk of acquiring HIV infection, other sexually transmitted diseases (STDs), or infections associated with drug injection, according to CDC surveys of high school students. Those behaviors include:
- Having premarital sex
- Using alcohol or drugs when they had sex, which may increase the likelihood of having unprotected sex
- Using injected illegal drugs
How To Information:
Public health experts suggest the following measures to help prevent HIV infection in young women:
- Sex education that includes information about AIDS and STDs.
- Access to safe sex products, such as condoms.
- Availability of understanding adults to consult, including parents, teachers, guidance counselors, healthcare professionals, and spiritual counselors such as ministers, priests, and rabbis.
Middle-Aged and Older Women
Eleven percent of all new U.S. AIDS cases are now in people over the age of 50. In the last few years, new AIDS cases rose faster in middle-aged and older people than in people under the age of 40.
In older women, sexual activity has been the most common cause of HIV infection, followed by infection from a blood transfusion before 1985. (U.S. blood banks began testing all donated blood for the presence of HIV in 1985. Today, there is little danger of getting HIV from transfusions in countries with good HIV blood screening programs.)
Need To Know:
Older women may not consider the possibility that they are HIV-infected because they don’t belong to a group commonly considered “at risk.” Furthermore, older women, unlike their younger counterparts, have not had the opportunity to learn about HIV in sex education classes.
Special concerns about HIV and AIDS in older women include:
- Faster disease progression. There is an age-related decline in the immune system’s disease-fighting ability. Older women with HIV usually become sick and die sooner than younger HIV-infected women.
- Diagnostic delays. Health professionals may have a more difficult time recognizing AIDS in older women because early symptoms – fatigue, confusion, a loss of appetite, and swollen glands – also are found in other illnesses common in older people.
- Treatment delays. Delays in diagnosis may mean that older women are not receiving timely treatment with medications to slow progression of the disease and prevent
opportunistic infections . - Drug interactions. Medications commonly used by older women, such as blood pressure drugs or hormone replacement therapy, can interact with drugs used to treat HIV and AIDS. To avoid such interactions, a physician should be made aware of all medications that a patient with HIV infection is taking.
Older women should educate themselves about behaviors that put them at risk for HIV infection and measures they can take to avoid becoming infected.
Women in Poverty
Demographic studies have shown that a disproportionate number of women diagnosed with HIV and AIDS, both in the United States and abroad, are economically disadvantaged. Poverty increases a woman’s vulnerability to
Poverty and injection drugs are importance forces driving the spread of HIV in women the United States, particularly in poor communities. This is because:
- Many women who acquire HIV infection sexually are infected through sex with an injection drug user.
- Female sex workers (prostitutes) generally have no knowledge of their clients’ HIV risk factors and are often unwilling or unable to insist on
condom use. - Female sex workers (prostitutes) often are exposed to violence, coercion, and abuse, further preventing them from being able to protect themselves from HIV infection.
How Does AIDS Affect Women?
Most people newly infected with the HIV virus show few, if any, symptoms for a few years. But during this asymptomatic period, HIV is actively multiplying, infecting, and killing cells in the immune system, particularly CD4+ T cells. People are very infectious during this early phase.
As the immune system weakens, symptoms begin to emerge.
Early Symptoms Of HIV Infection
Some people, but not all, develop symptoms within a month or two of exposure to HIV. Men and women may have a flu-like illness with such symptoms as:
- Fever
- Rash
- Headache
- Loss of appetite
- Swollen glands (enlarged lymph nodes)
- Achy muscles and joints
These early symptoms usually disappear within a week to a month. Most HIV-infected people who experience these early symptoms won’t see any more signs of the infection for at least a few years.
Later Symptoms Of HIV Infection
Usually, it takes about eight to nine years between the time of infection and the appearance of later symptoms, although this varies from person to person. These symptoms signal that immune system function is deteriorating, due to declining numbers of CD4+ T cells.
Not all people with HIV infection develop further symptoms. For those who do, however, symptoms may include:
- Persistent, enlarged lymph nodes
- Excessive fatigue
- Weight loss
- Frequent fevers
- Night sweats
- Chronic or frequent diarrhea
- Genital sores (sores around the penis or vagina)
Thrush (an infection of the mouth caused by Candida, a yeast-like fungus) and mouth lesions- Skin rash or flaky skin
- Joint stiffness and pain
- Bone pain
- Blurred vision
- Short-term memory loss
- Repeated bacterial, viral, or fungal infections
As the CD4+ T cell count continues to drop and the immune system deteriorates further, individuals may continue to experience the above symptoms as well as develop new ones.
There also are symptoms specific to women, such as gynecological problems.
What Symptoms Signal The Onset Of AIDS?
An HIV-infected person receives an
- A CD4+ T cell count of less than 200, and/or
- At least one of more than two dozen
opportunistic infections and conditions
In the United States, the most common AIDS-defining condition in both women and men is a lung infection called
Other AIDS-defining conditions include severe body wasting andCandida infection of the esophagus, windpipe, or lungs.
What Symptoms Are Specific To Women?
Women and men are not equally susceptible to HIV- and AIDS-related conditions.
- For example, men are eight times more likely than women to get the skin cancer known as
Kaposi’s sarcoma . - Some studies have shown that women with HIV infection are more likely than HIV-infected men to develop
Candidiasis in the esophagus or activeherpes simplex virus infections.
Gynecological problems occur more frequently and severely with HIV-infected women than in uninfected women. These problems include:
- Vaginal yeast infections
- Bacterial vaginosis (an imbalance of bacteria normally found in the vagina)
- Sexually transmitted diseases, including
gonorrhea, chlamydia infection, and trichomoniasis - Severe skin ulcers caused by herpes simplex virus
- Genital ulcers of unknown cause
- Human papillomavirus (HPV) infections, which can cause genital warts and can lead to cervical cancer
- Pelvic inflammatory disease that doesn’t respond to treatment
- Menstrual irregularities
Unique Issues For Older Women
Women over age 45 should remind their doctors about age-appropriate health screening. Doctors can sometimes be so focused on treating and managing HIV that they forget to deliver age-appropriate health screening that includes monitoring for all the conditions noted above.
Depression is also a common issue among older women. While obvious psychological and social factors can increase rates of depression among positive older women (including fear of disclosure and loneliness), there may also be a physiologic basis for depression.
Here’s why: After menopause, women produce less of the chemical serotonin. Low levels of this chemical are associated with depression, though this doesn’t necessarily mean that low levels cause depression. Hormone-replacement therapy may lessen incidence of depression by raising serotonin levels. However, more studies are needed to determine if this is a direct benefit of hormone-replacement therapy.
How Is HIV Infection Diagnosed in Women?
A blood test is used to confirm whether a woman has been infected with HIV. Any woman who has engaged in risky behavior, such as sharing drug-injecting equipment or having unprotected sexual contact with an infected person or with someone whose HIV status is unknown, should consider being tested.
A positive HIV test result does not mean that a person has AIDS. Not everyone who has HIV infection develops AIDS. Experts estimate that about half the people with HIV will develop AIDS within 10 years after becoming infected.
Early diagnosis of HIV infection is important for both men and women because:
- It allows people to seek treatment that will help suppress HIV’s attack on the immune system and prevent opportunistic infections.
- It alerts those who are infected that they could infect others.
Early detection is especially important for women who are sexually active. It helps women at risk for HIV infection who are planning a pregnancy or who are already pregnant take steps to reduce the risk of transmitting the infection to the baby.
How To Information:
Where is HIV testing available?
HIV testing is available at most hospitals, family planning clinics, sexually transmitted disease (STD) clinics, community health centers, drug treatment facilities, and doctor’s offices. Individuals can contact their local health department for testing centers in their area. In many states, it is possible to be tested anonymously.
Information about testing centers is also available by calling the CDC’s National AIDS Hotline. Testing centers will also provide counseling about HIV and AIDS and help people understand their test results.
Nice To Know:
Q: Is a home test kit for HIV available?
A: No approved HIV test kit will give you a result at home. There is a kit available that is designed for you to collect a sample of your blood at home. Then you send the sample to a laboratory where it is tested for
What Kinds Of Blood Tests Are Used?
The blood tests most commonly used to diagnose HIV infection work by measuring the levels of
- Enzyme immunoassay (EIA)
- Enzyme-linked immunosorbent assay (ELISA)
Western blot test
Usually, the first test that laboratories use to detect the presence of HIV antibodies is an EIA or the ELISA. If the first test produces a positive result (HIV antibodies appear to be present), then the more sensitive Western Blot test is used to confirm it.
EIA or ELISA tests take from one to two weeks to complete, depending on where the test is performed.
Why Is It Often Necessary To Repeat An HIV Test?
Although a negative result on an HIV blood test usually means that the person is not infected with the
Because of this delay between infection and the appearance of HIV antibodies, a person should be retested six months after the last possible exposure to HIV. It is also important to remember that a person who has been exposed to HIV can pass the virus to others even before HIV antibodies appear in the bloodstream.
What Should a Woman Do If She Tests HIV-Positive?
A woman who tests positive for HIV should take steps to protect her own health and the health of others. The CDC recommends that people with HIV infection:
- Promptly seek care from a physician or medical service, even if they feel well. Early treatment, preferably under the guidance of a doctor with experience treating people with HIV, can help slow damage to the immune system, prevent life-threatening conditions, and prolong life.
- Adopt a healthy lifestyle. Eating a balanced diet, exercising regularly, and getting enough sleep can help women with HIV stay healthy. Cigarette smoking, excessive alcohol consumption, and using illegal drugs such as cocaine can weaken the immune system.
How To Information:
A woman who learns she is HIV-positive should inform her sexual partner or partners, or people with whom she has shared drug-injecting equipment, and urge them to be tested and/or seek medical care for the infection.
There are many places where a woman can turn for information and support, such as:
- The CDC’s National
AIDS Hotline offers general information about treatments, practical advice on maintaining health, and referrals to local AIDS organizations and healthcare professionals who are knowledgeable about HIV and AIDS. - Publications and referrals are also available from the CDC’s National Prevention Information Network, which operates the National AIDS Clearinghouse.
How Does HIV Affect a Woman’s Birth Control Choices?
HIV-infected women who are using or plan to use birth control should consult with their physician or a family planning clinic for information about contraceptive methods.

The only birth control method that is considered highly effective in reducing the transmission of HIV and other STDs is the
Women should also be aware that some medications that are used to treat HIV and HIV-related
Federally funded programs are available that provide family planning services (including birth control information, condoms and other contraceptives, and physical examinations) for those who cannot afford them. Women can consult their city health department or family-planning clinic for more information about these programs.
Having Sex With an HIV-Negative Partner
An HIV-positive woman should inform an HIV-negative sexual partner about her HIV diagnosis, so that steps can be taken to safeguard her partner’s health and reduce future risk of HIV transmission. Such safeguards include “safer sex” practices-activities that reduce the risk of transmitting HIV and other sexually transmitted diseases to an uninfected partner.
Activities that pose no risk of HIV transmission include:
- Dry kissing and hugging
- Massaging each other
- Using a clean vibrator or
dildo (or one that has been covered with a new condom) on each other
Activities that are considered relatively safe, but which may pose some risk of HIV transmission include:
- Vaginal and anal sex with a properly used latex condom
- Oral sex with a latex barrier (a condom to cover the penis or a dental dam to cover the vagina)
- Inserting a finger or hand, covered by a latex glove, in a partner’s vagina or rectum
Having Sex With an HIV-Positive Partner
Even when a woman and her partner are both HIV-positive, safer sex practices are still needed to prevent each person from infecting the other with a different strain of HIV. These precautions are also needed to reduce the transmission of other sexually transmitted diseases, such as herpes or
HIV Infection and Pregnancy
About one-fourth of pregnant HIV-infected women in the United States who are not treated with the anti-HIV drug
How To Information:
A pregnant woman can greatly reduce the risk of infecting her baby if she takes AZT during her pregnancy. Because the risk of transmission increases with longer delivery times, the risk can be further reduced by delivering the baby by
HIV Infection and Breast-Feeding
HIV also may be transmitted from a nursing mother to her infant. Recent studies suggest that breast-feeding introduces an additional risk of
- Women who live in countries where safe alternatives to breast-feeding are readily available and affordable can eliminate the risk of transmitting the virus through breast milk by bottle-feeding their babies.
- In developing countries, however, where such safe alternatives are not readily available or economically feasible, breast-feeding may offer benefits that outweigh the risk of HIV transmission.
What Treatments Are Available For HIV and Aids?
When AIDS first surfaced in the United States, no drugs were available to combat the underlying immune deficiency, and few treatments existed for the opportunistic infections that resulted. Over the past 10 years, however, therapies have been developed to fight both HIV infection and its associated infections and cancers.
Although there is no treatment currently available that can cure people of HIV or AIDS, a number of therapies have been developed to help them stay healthier and live longer.
- Some medications target HIV itself, to reduce the virus’s assault on the immune system.
- Other treatments are used to treat or prevent specific opportunistic infections that threaten the health of people with HIV-damaged immune systems.
Need To Know:
Unfortunately, not all women with AIDS receive the best medical care, according to a recent five-city study. The study concluded that the main reason for this was women’s family obligations. In other words, many women look after their family’s health before taking care of themselves.
Treatments That Suppress HIV
Drugs that interfere with the activity of a retrovirus such as HIV are generally known as antiretrovirals. All antiretroviral medications currently approved to treat HIV infection target two viral enzymes used by the
Three classes of
- Nucleoside analog reverse transcriptase inhibitors (NRTIs).NRTIs interrupt an early stage of HIV replication by interfering with the activity of reverse transcriptase.
AZT (zidovudine), the first drug approved for treating HIV infection, is an NRTI, as arezalcitabine (ddC), didanosine (ddI), stavudine (d4T), lamivudine (3TC), and abacavir. - Non-nucleoside reverse transcriptase inhibitors (NNRTIs).NNRTIs also work by hindering the action of reverse transcriptase. This class of drugs includes delavirdine, nevirapine, and efavirenz.
Protease inhibitors . Protease inhibitors interrupt a later stage of viral replication. This class of drugs includes saquinavir, indinavir, ritonavir, nelfinavir, and amprenavir.
Studies have found that various combinations of antiretroviral drugs are more effective in suppressing HIV than antiretroviral drugs used alone. Experts refer to one common treatment approach, usually involving a protease inhibitor combined with two other antiretroviral drugs, as “highly active antiretroviral therapy” or HAART.
Drug combinations, or drug “cocktails,” also can help reduce the risk that drug-resistant HIV will develop. When drug resistance occurs, medications that initially succeeded in suppressing the replication of HIV in the patient’s body loose their effectiveness.
Antiretroviral drugs have side effects that can limit their use in some people.
- AZT, for example, may result in a loss of blood cells.
- Protease inhibitors can cause nausea, diarrhea, and other symptoms.
Treating AIDS-Related Conditions
Other drugs and therapies are used to prevent or treat opportunistic infections and other AIDS-related conditions:
Pneumocystis carinii pneumonia. People who develop this lung infection are generally treated with TMP/SMX (a combination of antibiotic drugs) or pentamidine. Doctors also prescribe these medications as preventive therapy for adult patients whose CD4+ T cell counts fall below 200.- Yeast infections in women. Physicians often prescribe a drug called
fluconazole to treat yeast and other fungal infections.Fluconazole also can safely prevent vaginal and esophagealcandidiasis without development of drug resistance. - Severe skin ulcers caused by
herpes simplex virus infection.Skin ulcers sometimes respond to an antiviral medication,acyclovir. - Pelvic inflammatory disease. PID is treated with antibiotics. Women with mild cases may be treated on an outpatient basis. HIV-positive pregnant women suspected of having PID are usually hospitalized, treated with intravenous antibiotics approved for use during pregnancy, and monitored closely.
- HIV-related wasting.Megestrol acetate (Megace) is often prescribed for HIV-associated wasting, but it can cause significant irregular vaginal bleeding in women. Another drug, nandrolone, may not have these side effects and is currently undergoing drug trials.
Kaposi’s sarcoma and other cancers. Cancers are treated with radiation, chemotherapy, or injections of alpha interferon, a genetically engineered, naturally occurring protein.
For further information about radiation, go to Radiation Therapy
Need To Know:
Many of the gynecologic complications that HIV-positive women experience also affect women who are not infected with HIV. However, these problems tend to be more frequent, are more serious, and are more difficult to treat in women whose immune system is compromised. At the same time, gynecologic complications can further damage the immune system.
Since many of these complications do not immediately cause symptoms, regular exams are crucial, even when a woman is feeling well. Diagnosis and treatment at early stages is critically important in preventing a gynecologic complication from progressing.
What Are Some Of The Problems With AIDS Drug Therapy?
AIDS drugs do not cure the condition, but they help to manage it and postpone life-threatening complications. However, there are problems with AIDS drug therapy:
- Side effects of drugs are a major concern in treatment.
- Another major problem is the cost of the drugs used in treating AIDS. AIDS patients in the United States depend on insurance and government grants to obtain them. The high price of these drugs makes it difficult for third-world countries, which have major AIDS epidemics, to afford to distribute them.
Since antiviral drugs have so far not been curative, the hope is to find a vaccine. The technology for vaccine development is present, and serious efforts are being made to find one.
How Can The Psychological Impact Of AIDS Be Managed?
When people learn they have tested positive for the HIV virus, they may experience a number of stressful psychological reactions. Depression and anxiety leading to panic attacks may require the help of an adviser or psychological therapist. Counseling services are available in most HIV clinics. Group therapy sessions with other HIV-positive people may also be helpful in managing feelings of stress and guilt.
People with AIDS who show signs and symptoms of organic central nervous system involvement, such as confusion and memory loss, need particular support. In their cases there is a need for additional medical and psychiatric intervention.
Antidepressant drugs should be used under the advice of a specialist in case of a severe depressive episode. HIV-infected people may take antidepressant drugs, but they are usually more sensitive to their side effects.
What About Newer AIDS Treatments?
Medical researchers are working to develop new drugs to keep HIV replication in check, as well as medications and methods to treat or prevent opportunistic infections and other HIV-related conditions.
For example, research under way includes studies of treatments for:
- Human papillomavirus (HPV) infections. A precancerous condition associated with HPV, cervical intraepithelial neoplasia (CIN), is more common and more severe in HIV-infected women. One study sponsored by the National Institute of Allergy and Infectious Disease (NIAID) is assessing drugs to determine if they can prevent recurrences of precancerous tissues in the cervix or stop precancerous cells from progressing to cervical cancer
- Idiopathic genital ulcers. Although these ulcers are sometimes confused with those caused by herpes simplex virus, the cause of idiopathic genital ulcers is unknown. Idiopathic genital ulcers are a unique manifestation of HIV and have no proven treatment. Researchers are evaluating the effect of the drug thalidomide (proven effective in treating mouth ulcers in patients with HIV) on idiopathic genital ulcers in HIV-infected women.
About Clinical Trials
Some people with HIV and
Clinical trials are conducted in humans only after they are tested in laboratories and in animal studies. They are designed to develop better treatments for people while giving current patients a chance to benefit from new treatments that may be more effective.
- For information about studies of new HIV therapies, call the AIDS Clinical Trials Information Service at 1-800-TRIALS-A (1-800-243-7012 for TDD/deaf access).
- For federally approved treatment guidelines on HIV/AIDS, call the HIV/AIDS Treatment Information Service at 1-800-HIV-0440 (1-800-243-7012 for TDD/deaf access).
What is the Long-Term Outlook for Women With AIDS?
Early diagnosis and treatment with drugs that suppress the activity of HIV and prevent or treat opportunistic illnesses can help women who are HIV-positive live longer and healthier lives.
Women living with HIV or AIDS also benefit from a supportive community that includes healthcare workers, friends, and family. A loving environment can encourage a woman living with HIV to maintain a positive approach toward her treatment and live a full, productive life.
What Can Women Do To Prevent HIV Infection?
Since no vaccine for HIV is available, the only way to prevent infection by the virus is to avoid behaviors that place a person at risk for infection, such as sharing needles and having unprotected sex.
Prevention is the key to personal protection against HIV and AIDS. Being aware of behaviors that increase the risk of infection and taking preventive measures can substantially reduce a person’s likelihood of becoming infected with HIV.
Prevention involves:
- Safer sex practices
- Drug use and limiting HIV exposure
- Minimizing HIV exposure from medical procedures
Safer Sex Practices
The CDC recommends complete sexual abstinence as a foolproof way to prevent sexually transmitted HIV. A monogamous sexual relationship between two uninfected individuals also limits the risk of HIV exposure through sex – as long as both partners are completely faithful and avoid nonsexual exposure to HIV, such as through injection drugs.
Safer sex practices should be followed during sexual contact with any partner, male or female, who is HIV-positive or whose sexual history is unknown. An individual who is infected with HIV is able to transmit the virus:
- Even if he or she has no symptoms of the infection
- Immediately after he or she has become infected
How To Information:
Safe sex practices involve creating a barrier between a person’s mucous membranes (or any cuts or breaks in the skin) and his or her partner’s blood, semen, or vaginal secretions. Such barriers include:
- Condoms, with or without
spermicide Dental dams (squares oflatex , originally used for dental work, now commonly recommended for safe oral sex)- Latex gloves
Most condoms are made from latex rubber. Using latex condoms, correctly and consistently, can greatly reduce a person’s chance of acquiring or transmitting HIV and most STDs. There is no scientific evidence demonstrating that spermicides (which are used for their contraceptive properties) offer protection against HIV infection.
Not all condoms are alike.
- Lambskin condoms, which are porous and may allow HIV and other viruses to pass through them, are not recommended for protection against HIV and other STDs.
- Polyurethane condoms, on the other hand, may provide an alternative for people who are allergic to latex.
The female
Need To Know:
Experts caution that oil-based lubricants should never be used with latex condoms or the other latex barriers, as these may erode the material and destroy the barrier. Recommended “condom-compatible” lubricants are water-based, such as
Sexual activities that do not involve contact with blood or other bodily fluids, such as hugging, “dry” or closed-mouth kissing, and use of non-shared
Drug Use And Limiting HIV Exposure
People who use injection drugs risk exposure to HIV if they share needles and syringes with others. HIV in the blood residue from an infected person can be transmitted directly into the bloodstream of the next person using the injecting equipment.
Health authorities recommend that people who use illegal drugs seek treatment to help them stop. Those who cannot end their drug use are advised to avoid sharing drug injection equipment with others.
Programs that distribute clean needles to injecting drug users have helped to lower the incidence of HIV infection among these people.
Minimizing HIV Exposure From Medical Procedures
HIV has been transmitted through transfusions of contaminated blood and blood components. In the United States, several thousand surgical patients and others became HIV-infected through receiving contaminated blood, most of them early in the AIDS epidemic.
Since 1985, however, blood banks have added new safeguards to their procedures to ensure that donated blood does not present an HIV risk. These measures include various heat-treating techniques and screening donated blood for evidence of HIV. Blood from potential donors who are determined to have risk factors for HIV transmission is also discarded.
Today, the risk of acquiring HIV infection from blood transfusions is extremely small. People who are scheduling elective surgery can reduce the risk even further by banking some of their own blood before the surgery. This is known as autologous blood donation.
HIV transmission as a result of other medical procedures is rare, although accidental sticks with contaminated needles have occurred, mostly among healthcare workers.
Dentists, hygienists, and other healthcare professionals are required to wear protective latex gloves to avoid the transmission of viral infections such as HIV.
Frequently Asked Questions: AIDS And Women
Here are some frequently asked questions related to AIDS And Women.
Q: What if I’m attracted to someone I don’t really know? What should I do?
A: Know the sexual history and health status of partners. Avoid anonymous sexual contact and learn about safe sex practices, such as the use of condoms.
Q: Are my children going to get AIDS if I have it?
A: Research indicates that
Q: Is an AIDS test required of new job applicants and/or employees?
A: Probably not. In fact, under most state laws, employers cannot ask whether applicants or employees have AIDS – only if they can do the job.
Q: Should I avoid sharing personal hygiene items, like razors or toothbrushes?
A: Yes. These devices might be contaminated with blood. However, this is an unlikely mode of transmission for the AIDS
Q: Does everyone who has AIDS die from it?
A: When scientists first recognized AIDS in 1981, most people died within a year or two. Now, with numerous drugs available to help suppress HIV’s attack on the
Q: How can a person tell if she is infected with HIV?
A: A blood test can determine whether or not a person is infected with HIV. The most commonly used test detects
Q: Can I keep my test results private?
A: People can have the procedure done at HIV testing centers that offer anonymous HIV testing.
Q: Can HIV be spread through kissing?
A: Although studies have found tiny amounts of HIV in the saliva of some people with HIV, researchers have found no evidence that HIV is spread to other people through kissing. However, the CDC recommends against “French” or open-mouthed kissing because of the possibility of contact with blood if the people kissing have any cuts or sores in the mouth.
Q: Can HIV be transmitted during oral sex?
A: Although the risk of infection during oral sex is considered lower than during vaginal or anal intercourse, HIV may be transmitted during oral sex through contact with vaginal secretions, semen, pre-ejaculation fluid, and blood.
Q: Is a home test kit for HIV available?
A: No approved HIV test kit will give you a result at home. There is a kit available that is designed for you to collect a sample of your blood at home. Then you send the sample to a laboratory where it is tested for HIV.
Q: How likely is an HIV-positive woman to infect her baby?
A: Approximately one-quarter to one-third of all untreated pregnant women infected with HIV will pass the infection to their babies during pregnancy or childbirth. But this risk is significantly reduced if the mother is treated with
Q: Can HIV be transmitted in breast milk?
A: HIV can be transmitted from a nursing mother to her infant through breast milk. Women who live in countries where safe alternatives to breast-feeding are readily available and affordable can eliminate the risk of transmitting the virus through breast milk by bottle-feeding their babies. In developing countries, however, where such safe alternatives are not readily available or economically feasible, breast-feeding may offer benefits that outweigh the risk of
Q: How effective are
A: Health authorities say that latex condoms are highly effective when used consistently and correctly. The Centers for Disease Control and Prevention recommends using latex condoms (or
Putting It All Together: AIDS And Women
Here is a summary of the important facts and information related to AIDS And Women.
- AIDS (acquired immunodeficiency, or immune deficiency, syndrome) is an advanced stage of a viral infection that attacks the body’s disease-fighting
immune system . HIV (the human immunodeficiency virus) is the infectious agent that is the cause of AIDS.- Women can become infected with HIV through unsafe sexual contact with individuals infected with the
virus , by sharing drug-injecting equipment, or (more rarely) by receiving a bloodtransfusion from an HIV-infected blood donor. - Women can prevent HIV infection through safer sex practices and avoiding contact with blood from an infected person.
- Early symptoms of HIV infection include excessive fatigue, significant weight loss, and frequent infections.
- Gynecological problems occur more frequently and are more severe in HIV-infected women than in uninfected women.
- HIV/AIDS testing is available anonymously through clinics and requires a blood sample.
- Not everyone who has HIV infection develops AIDS.
- An HIV-infected woman can take precautions to substantially reduce the risk of infecting her baby during pregnancy or childbirth.
- A number of drugs are available to help HIV-infected individuals live longer and healthier lives
Glossary: AIDS And Women
Here are definitions of medical terms related to AIDS And Women.
AIDS: Acquired immunodeficiency (or immune deficiency) syndrome, an advanced stage of a viral infection caused by the human immunodeficiency virus (HIV)
Antibodies: Proteins produced by the immune system to fight infectious agents, such as viruses
Antigen: A substance that stimulates the production of antibodies
Antiretroviral drugs: Chemicals that inhibit the replication of retroviruses, such as HIV
Asymptomatic: Having no symptoms
Autoimmune disorder: Illness that results when the immune system attacks an individual’s own tissues or cells
AZT: An antiretroviral drug used to treat HIV infection; also called zidovudine
B lymphocytes: White blood cells that mature in the bone marrow and produce antibodies; also called B cells.
Bisexual: A person who is attracted to and/or has sex with both men and women
Cesarean section: The delivery of a baby through a surgical incision through the abdominal wall and the uterus
Candidiasis: An infection, usually caused by the yeastlike fungusCandidaalbicans, that occurs in the mouth, vagina, and other moist areas of the body
CD4: A protein displayed on the surface of a certain human immune cells. HIV recognizes, attaches to, and infects cells bearing CD4 on their surface
Cervical intraepithelial neoplasia (CIN): A precancerous condition of the cervix (the bottom of the uterus) that is more common and more severe in HIV-infected women.
Chlamydia: A group of bacteria that includes a sexually transmitted bacterium, Chlamydiatrachomatis; in women, the infection can cause a vaginal discharge and is a major cause of pelvic inflammatory disease
Condom: A sheath, usually made of latex, designed to cover the penis during sexual intercourse to help prevent pregnancy and reduce the risk of sexually transmitted diseases, including HIV
Dendritic cells: Immune cells that may bind to HIV after sexual exposure and carry the virus from the site of infection to the lymph nodes
Dental dams: Squares of latex, originally used for dental work, now commonly recommended for safe oral sex
Dildo: A sex toy, usually made of silicone or rubber, that is inserted into the vagina or the anus
Enzyme immunoassay (EIA): A test used to detect HIV antibodies in a blood sample
Enzyme-linked immunosorbent assay (ELISA): A test used to detect HIV antibodies in a blood sample
Fluconazole: A drug commonly used to treat yeast infections such as oral, esophageal, and vaginal candidiasis
Gonorrhea: A sexually transmitted disease caused by the bacteriumNeisseriagonorrhoeae.
Herpes simplex virus: Human viruses responsible for blister-like lesions around the mouth and lips, the anus, or the genital area
Heterosexual: A person who is sexually attracted to and/or has sex with someone of the opposite sex
HIV: The human immunodeficiency virus, a retrovirus recognized as the cause of AIDS
Homosexual: A person who is sexually attracted to and/or has sex with someone of the same sex
Human papillomavirus (HPV): A family of viruses that cause warts, including anal and genital warts.
Idiopathic genital ulcers: Lesions on the genitals of unknown cause seen HIV-infected individuals.
Immune system: The cells and tissues in the body that fight infection and disease
Immunity: The body’s ability to resist infection
Injection drugs: Drugs such as heroin or morphine that are injected through a syringe and needle into a vein
Kaposi’s sarcoma: A cancerous tumor that arises from blood vessels in the skin, which occurs in some people with HIV and AIDS
K-Y Jelly: A water-based lubricant used with latex materials such as condoms
Latex: A synthetic rubber used in products such as gloves and condoms, to provide a barrier to infection
Lymph nodes/lymph glands: Small, round or oval bodies connected by a network of vessels; they help remove bacteria and foreign particles from the circulation, and play a role in the body’s immune defenses
Lymphocytes: White blood cells that play a key role in the body’s disease-fighting immune response
Macrophages: Specialized white blood cells that play many roles in the immune response, including engulfing and digesting bacteria and other microbes, alerting other immune cells, and producing chemicals needed for immune responses to disease threats
Opportunistic infections: Infections (rarely seen in healthy people) that that occur when a person’s immune system is weakened due to HIV, cancer, or drugs that suppress the body’s immune response
Pelvic inflammatory disease (PID): A gynecologic condition caused by infection of a woman’s reproductive organs; it may cause severe abdominal pain and sterility
Phagocytosis: The process by which macrophages and other specialized cells engulf and digest of bacteria and other foreign particles
Pneumocystis carinii pneumonia: A type of pneumonia (lung inflammation) caused by a microbe called Pneumocystiscarinii, seen in people with impaired immunity
Protease inhibitors: Drugs that suppress HIV replication by interfering with an HIV enzyme called protease
Reverse transcriptase: An HIV enzyme that the virus requires to reproduce itself
Sex toys: Devices used for sexual pleasure, such as vibrators and dildos
Sexually transmitted diseases (STDs): Diseases caused by infectious agents that are transmitted through sexual contact, such as HIV/AIDS, chlamydia infection, syphilis, and gonorrhea
Spermicide: A substance that deactivates sperm cells and is used for birth control
T lymphocytes: A family of specialized white blood cells that help orchestrate the body’s immune responses and attack cells that are infected or cancerous
Thrush: Oral candidiasis, an infection of the mouth caused by caused by the yeast-like fungus Candidaalbicans
Transfusion: The injection of whole blood, plasma, or another solution into a patient’s bloodstream
Virus: A disease-causing microbe that can replicate only in the living cells of other organisms
Western blot: A test used to diagnose HIV infection by detecting antibodies to HIV in a person’s blood; this test is commonly used to confirm a less-sensitive HIV antibody test
Additional Sources Of Information: AIDS And Women
Here are some reliable sources that can provide more information on AIDS And Women.
The U.S. Centers for Disease Control and Prevention
1-800-311-3435
U.S. National Library of Medicine Web site
AIDS.org, a nonprofit organization designed to inform and educate using the Web
AIDS Legislative Update and Resources, a Web site designed to provide the latest information about legislative action related to AIDS.
http://www.house.gov/pelosi/aids.htm
Centers for Disease Control AIDS Clearinghouse
Phone: 1-800-458-5231
The clearinghouse offers free government publications and information about resources.
National Institute of Allergy and Infectious Diseases (NIAID),
The NIAID, which is part of the National Institutes of Health, will respond to written requests for information on AIDS research and clinical trials of promising therapies.
Information About
National AIDS Hotline operated by the Centers for Disease Control
1-800-342-AIDS
1-800-344-SIDA (for Spanish)
1-800-AIDS-889 (TTY)
The hotline operates 24 hours a day, seven days a week. It offers general information and local referrals.
Support Groups for HIV-Positive Women
Women Alive
National Women’s Health Network
1-202-347-1140
Project Inform Hotline (Treatment Information)
1-800-822-7422
Women Being Alive (Newsletter)
1-214-667-3262
Women Organized to Respond to Life Threatening Disease (WORLD)- (Newsletter)
1-510-658-6930
For People Over 50
American Association of Retired Persons (AARP), Social Outreach and Support (SOS)
Phone: (202) 434-2260
The AARP/SOS program has information on HIV and AIDS and its impact on midlife and older adults.
Social Security Administration
Contact local office or call (800) SSA-1213
Social Security has two disability benefit programs that provide financial assistance to eligible AIDS patients.
Seniors in a Gay Environment (SAGE)
Phone: (212) 741-2247
SAGE provides HIV/AIDS information and referrals for men and women over the age of 50.
Information About Studies Of New HIV Therapies
HIV/AIDS Clinical Trials Information Service
1-800-TRIALS-A
1-800-243-7012 (TDD/Deaf Access)
HIV/AIDS Treatment Information Service
1-800-HIV-0440
1-800-243-7012 (TDD/Deaf Access)
